Q-Tip Test: Diagnosing Neuropathic Facial Pain
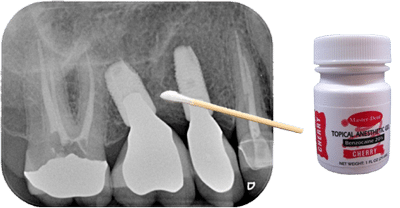
The Q-tip test is a simple but powerful clinical technique used by orofacial pain specialists to help determine whether unexplained facial or oral pain is nerve-based (neuropathic) rather than dental or musculoskeletal in origin. It can help identify trigger zones, guide further diagnostic steps, and steer patients toward appropriate treatment. If a Q-tip causes pain, it is called allodynia, which is a painful response to a non-painful stimulus such as when you get a sunburn and touching your skin hurts.
What Is the Q-Tip Test?
The Q-tip test involves gently touching or applying light pressure to areas of the face or oral tissue with a cotton swab (Q-tip) to determine whether the contact reproduces the patient’s pain. Because neuropathic pain is often triggered by light touch or pressure, this assessment can provide important clues about the nerve involvement in a patient’s symptoms.
How the Q-Tip Test Is Performed
- Confirm pain is not dental in origin: Before performing the test, dental causes such as infection, cracked teeth, or periodontal disease should be ruled out.
- Patient-reported pain location: Ask the patient to describe exactly where the pain occurs — it can help to have them point with the Q-tip itself.
- Light touch assessment: Gently stroke the reported area with a Q-tip, as if you were using a paintbrush with a light touch, to see if this elicits the familiar pain.
- Firm pressure assessment: Apply gentle, firm pressure on several areas around the painful site with the Q-tip to see if deeper mechanoreceptors trigger the pain.
- Anesthetic verification: If pain is replicated, a topical anesthetic such as 20% benzocaine can be applied to the area. Wait a few minutes and repeat the test. A reduction or elimination of pain supports the diagnosis of neuropathic pain.
The Pain is Temporarily Relieved – What Next?
If odontogenic sources have been excluded and any of these anesthetic approaches significantly reduce or eliminate the pain, the findings are consistent with a neuropathic pain. Specifically, it is a peripheral neuropathic pain involving the trigeminal nerve. If the pain was due to any type of trauma in the painful area, it is called post-traumatic trigeminal neuropathic pain (PTNP).
Next Steps After a Positive Q-Tip Test
If the Q-tip test suggests that pain is neuropathic:
- A detailed orofacial pain evaluation is usually recommended.
- Additional sensory testing or imaging may help clarify the diagnosis.
- Management may include targeted medications, nerve blocks, and individualized pain control strategies.
- Treatment will likely include a neurosensory stent for PTNP.
- Topical medication, such as a 50/50 mix of 0.025% capsaicin and 20% benzocaine, is applied inside the stent every two hours.
Why The Q-tip Test Matters
Many patients with chronic facial pain have been to multiple practitioners without a clear diagnosis. Pain originating from nerve dysfunction doesn’t always show abnormalities on dental X-rays or routine exams, and misdiagnosis can lead to unnecessary procedures. Orofacial pain specialists use tools like the Q-tip test as part of a comprehensive pain evaluation strategy to distinguish nerve pain from dental pathology or temporomandibular sources.
The Pain is Not Temporarily Relieved – What Next?
If repeated attempts with local topical anesthetic, tissue infiltration, or nerve blockade do not reduce the pain response, this may suggest that the pain is centralized — meaning the nervous system itself is sensitized — rather than arising from a peripheral trigger zone.
In cases involving the maxillary (upper) arch, an additional diagnostic and therapeutic step may include a sphenopalatine ganglion (SPG) block, which can be performed in the office. This may be done using a transnasal catheter technique, such as a Sphenocath, delivering local anesthetic to the same side of the pain. When an SPG block provides meaningful relief, it could stop the pain cycle. If the pain returns in a short amount of time, it may be repeated for 6 weeks to achieve longer-lasting symptom reduction.
