Signs and Symptoms of Myofascial Pain
Myofascial pain has been described as a dull, aching or burning muscle pain, soreness or numbness frequently characterized by a sensation of referred pain. Referred pain is a pain stimulus originating in one part of the body being felt in another muscle or muscle group.

Myofascial trigger points weaken the muscle in which they are present. The muscle experiences a constant state of contraction as the active trigger point tenses the muscle fiber, creating a taut band of muscle tissue. This taut band can become hard and rope-like and feels painful or stiff for the individual experiencing it. The affected muscles may have restricted motion and become quickly fatigued.
The pain associated with myofascial pain differs from other painful conditions, such as fibromyalgia, primarily in the way that it is experienced in a localized muscle or region of the body. However, myofascial symptoms may spread to other areas. An active trigger point or series of trigger points may cause adjacent muscles to become overworked, promoting the creation of new trigger points.
The sign of a myofascial trigger point is a focused point of tenderness or pain felt when pressure is applied. Pressure to a trigger point made with a finger may also cause a sensation of shooting pain along nearby muscles, such as from the back to the neck or shoulders. The trigger point feels like a hard knot of tissue to the touch, however it may not be apparent to the untrained observer because trigger points can be present deep within a muscle. A physical examination by a doctor is often required to uncover all present myofascial trigger points.
During a physical examination of a patient experiencing muscle pain, the doctor will typically ask a number of questions to help diagnose the underlying condition. Potential questions include:
- Does your job or hobbies require you to perform repetitive tasks?
- Have you recently been injured?
- What symptoms are present?
- What areas are experiencing the most pain?
- Do symptoms become worse during a certain time of day?
- Do symptoms become better or worse as a result of anything?
- How long have symptoms persisted?
- Are symptoms continuous or intermittent?
- Are any activities limited by symptoms?
Diagnosing Myofascial Pain
A diagnosis of chronic myofascial pain means that myofascial trigger points are the primary source of pain symptoms. Unfortunately, myofascial pain can mimic a variety of other conditions. For example, myofascial pain symptoms may be incorrectly attributed to headaches, arthritis, temporomandibular joint disorder (TMJD), or fibromyalgia, among a number of other pain conditions. Likewise, a medical provider may mistakenly overlook a myofascial pain diagnosis if a patient is also suffering from another pain-causing condition such as those listed above. For these reasons and the fact that myofascial pain is a poorly understood disorder, chronic myofascial pain disorder can be a difficult condition to diagnose.

During a physical examination of a patient experiencing muscle pain, the doctor will typically ask a number of questions to help diagnose the underlying condition. Potential questions include:
- Does your job or hobbies require you to perform repetitive tasks?
- Have you recently been injured?
- What symptoms are present?
- What areas are experiencing the most pain?
- Do symptoms become worse during a certain time of day?
- Do symptoms become better or worse as a result of anything?
- How long have symptoms persisted?
- Are symptoms continuous or intermittent?
- Are any activities limited by symptoms?
A doctor can identify trigger points located along muscle fibers by physically examining a patient’s musculature via palpation, or touch. Gentle finger pressure is applied along muscles, with the doctor looking for tight areas while watching the patient’s reaction for signs of increased sensitivity in an area. A muscle twitch or patients flinching from pain are potential signs. If it is determined that there is a focal point or points of pain within muscles, a doctor may recommend additional tests or procedures to rule out other possible causes of muscle pain. Palpation is the most common process of myofascial pain diagnosis.
What is Myofascial Pain?
Chronic myofascial pain (CMP) is a chronic pain disease characterized by trigger points in the musculature causing pain in distinct areas of the body. Pain symptoms of CMP can be severe and debilitating. While much of the underlying mechanics of myofascial pain is not clearly understood, research suggests that symptoms are derived from the existence of trigger points within muscles, which are activated by injury or repetitive strain to muscles. It is generally understood that while one trigger point may be responsible for an experience of myofascial pain, it is more commonly a network of several trigger points that contribute to pain in a given region.
The defining clinical definition of myofascial pain is an active pain trigger point, experienced as a focused point of tenderness within a muscle. Pain associated with myofascial pain is usually experienced as dull aching of a muscle and the associated muscle group. Referred pain, or pain experienced at a site adjacent or not near the originating trigger point, is also common.

An estimated 44 million Americans suffer from myofascial pain problems, and trigger points have been associated with an estimated 30 percent of pain problems in American pain complaints. Research suggests that myofascial pain triggers are a potential component of tension-type headaches, back pain, postural pain and other pain conditions.
Further studies suggest that most individuals have trigger points within their musculature, however for 45 percent of women and 55 percent of men, these trigger points are asymptomatic.
Chronic myofascial pain symptoms can be mistaken for a large number of other disorders, so a thorough physical examination is required for proper diagnosis of this largely not understood disease.
Chronic myofascial pain is a complex but manageable disease. Professional attention can help narrow down the causes of chronic pain and make a positive diagnosis of CMP based on physical examination and additional procedures to rule out alternative sources of a patient’s pain symptoms. Several treatment options, including physical therapy, oral appliances, and medications, can be leveraged as part of a comprehensive management plan.
The jaw movement animation was developed by a medical illustrator under the guidance of Dr. Hirschinger.
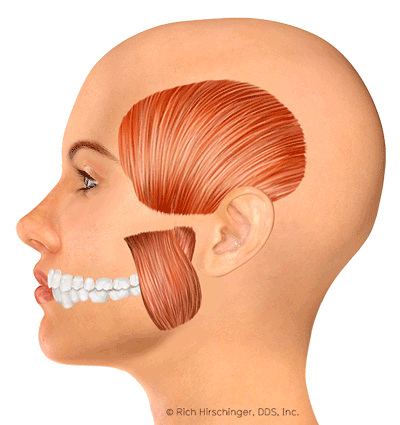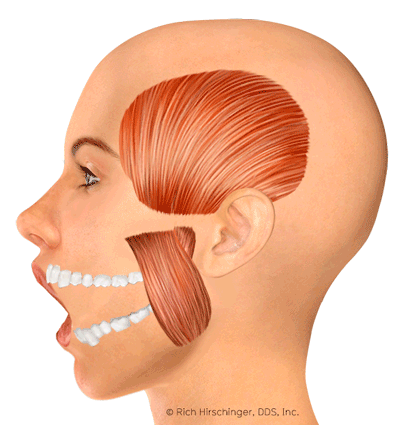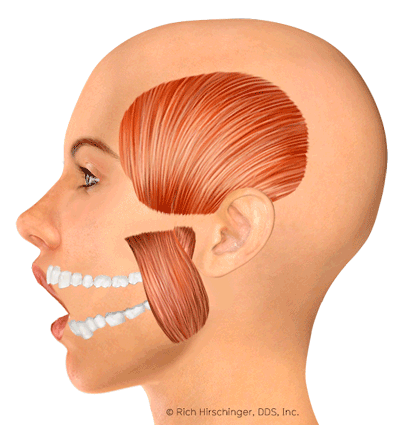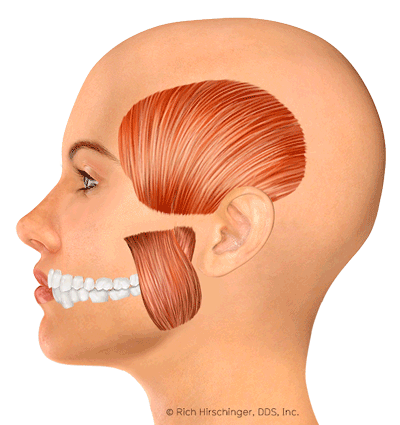
Foods and Habits to Avoid with Facial Muscle Pain
When something in your body is causing pain when it moves, it is best to minimize the movement of that body part. When it comes to jaw pain, it is not so easy to do since you have to eat, and you have to speak, and both of those movements involve moving your jaw. However, you can limit the amount of movement of your jaw so that you are not using the muscles that are causing your pain by choosing foods that do not require a lot of chewing, and avoiding habits that make the muscles work.
Foods to Avoid with Facial Muscle Pain
Some of the foods to avoid might seem obvious and some not so obvious. One of the foods that many people are surprised to learn that they should not eat is salad. When you think about it, you have to do a lot of chewing to eat a salad.
Generally you should avoid foods that are chewy, crunchy, hard, and sticky, and any food that requires you to open wide to bite into such as whole apples, submarines sandwiches, double deck deli sandwiches, a Double Double, etc.
This is clearly a partial list but it should give you a good guide to what types of food you should not eat in order to give your facial muscles as much of a rest as possible:
- Abba Zabba
- Apples
- Bagels
- Baguettes
- Caramels
- Carrots (raw)
- Celery
- Chewing gum
- Corn chips
- Corn on the cob
- French bread

- Gummy bears
- Hard candy – since we all know that no one can just suck on a hard candy without biting into it
- Hard rolls
- Ice
- Jawbreakers
- Jelly beans
- Licorice
- Look bar
- Now and Laters
- Nuts
- Peanut brittle
- Pizza crusts
- Popcorn
- Pretzels
- Raw vegetables – cooked vegetables are fine but they should be very soft
- Salads
- Snickers
- Skittles
- Starburst
- Sugar Babies
- Taffy
- Toffee
- Tootsie rolls
- Tortilla chips

Foods to Avoid with Facial Muscle Pain
It is important to not chew your nails, bite your lips or cheek, or bite on items with your teeth such as pens, pencils, bobby clips or any other object that causes your jaw muscles to make small repetitive movements.

Life with Myofascial Pain
An individual with chronic myofascial pain may approach their condition with a multi-part approach such as treating myofascial trigger points, managing ongoing pain, and reducing any contributing factors of the condition.
In order to treat the underlying mechanisms causing a patient’s myofascial pain, it’s important that the person take an active role in his or her treatment. A patient should take care to follow recommendations made by a doctor by doing exercises and movement programs at home and conducting self-therapy on trigger points.

Along with following the prescribed treatment regimen, a myofascial pain sufferer should remove potential co-factors of the condition from his or her life. This includes having an ergonomic evaluation of the workstation and other regular activities and making any recommended adjustments that may improve the quality of sleep and overall physical health.
Regular exercise can help a patient better cope with pain and strengthen muscles around the affected area to reduce the likelihood of additional myofascial trigger point creation. Quality restorative sleep, and a healthy and balanced diet can help the body better manage pain. And reducing stress through meditation, journaling, social interactions and other means can help relax muscle tension.
A patient can gain peace of mind helpful in coping with the condition by becoming educated about the causes and treatments of myofascial pain. Support groups and educational classes are offered by organizations such as the American Chronic Pain Association, comforting those affected by myofascial pain with assistance, advice and encouragement from others living with similar challenges. Speaking with dependable and trustworthy friends, family and colleagues can help both the patient and their loved ones better understand each other and more easily support one another through difficult periods.
Myofascial pain can have a strong impact on a person’s lifestyle, behavior and mood. An active treatment effort, the elimination of contributing factors and a supportive network can help relieve some of the distress of life with chronic myofascial pain.
