Muscles that Refer Pain and/or Sound into the TMJ/Ear
What “TMJ” Really Means — and Why It Is Not a Diagnosis
Many people say they have “TMJ,” but TMJ actually stands for the temporomandibular joint—an anatomical structure, not a diagnosis. The temporomandibular joint connects the lower jaw (mandible) to the temporal bone of the skull and allows the jaw to open, close, and move smoothly during talking, chewing, and swallowing.
Breaking down the term:
- T = Temporal bone (part of the skull)
- M = Mandible (the lower jaw)
- J = Joint (where the jaw and skull connect)
Because everyone is born with two temporomandibular joints—one on each side—saying “I have TMJ” is similar to saying “I have a knee joint.” The more accurate term when pain or dysfunction is present is temporomandibular disorder (TMD) or, more specifically, a diagnosis describing the true source of pain, such as jaw muscle pain, joint inflammation, disc displacement, osteoarthritis, etc.
Why the Temporomandibular Joint Is Unique
The temporomandibular joint is one of the most complex joints in the human body. It is the only joint that must function as a coordinated pair—both the left and right joints must work together for normal jaw movement. It is also unique because it performs two distinct types of motion:
- Hinge movement (rotation) for opening and closing
- Translational movement (sliding) for wider opening and forward movement of the jaw
You can explore these mechanics in more detail on the TMJ animation page.
Most “TMJ Pain” Is Actually Muscle Pain
Although the temporomandibular joint can be a source of symptoms, the majority of what patients call “TMJ pain” is actually jaw muscle pain. Overuse of the jaw-closing muscles—often from clenching, grinding (bruxism), stress, chewing gum, or prolonged dental procedures—can lead to muscle fatigue, tightness, and referred pain that mimics joint pathology.
Understanding Referred Pain Patterns
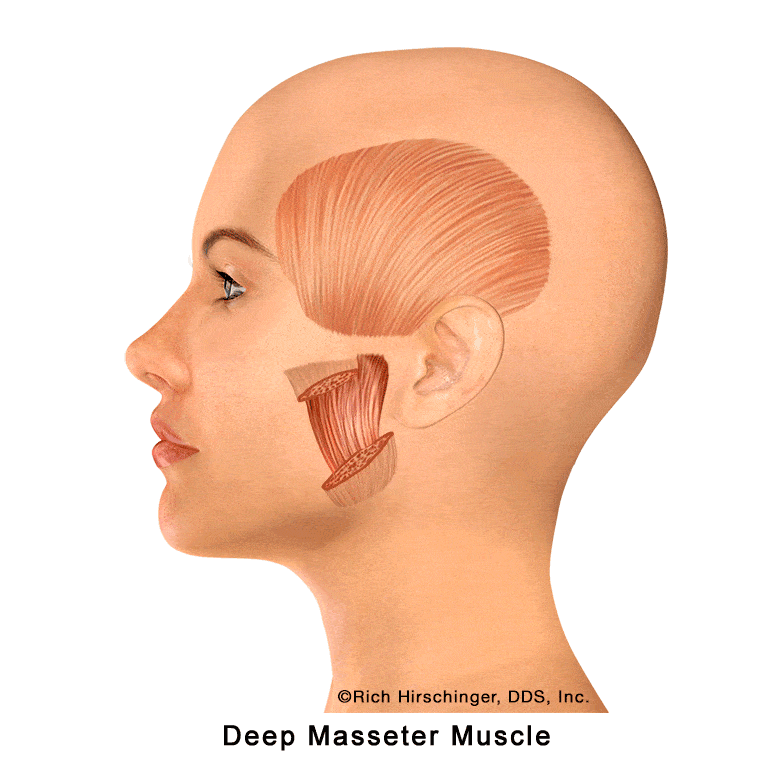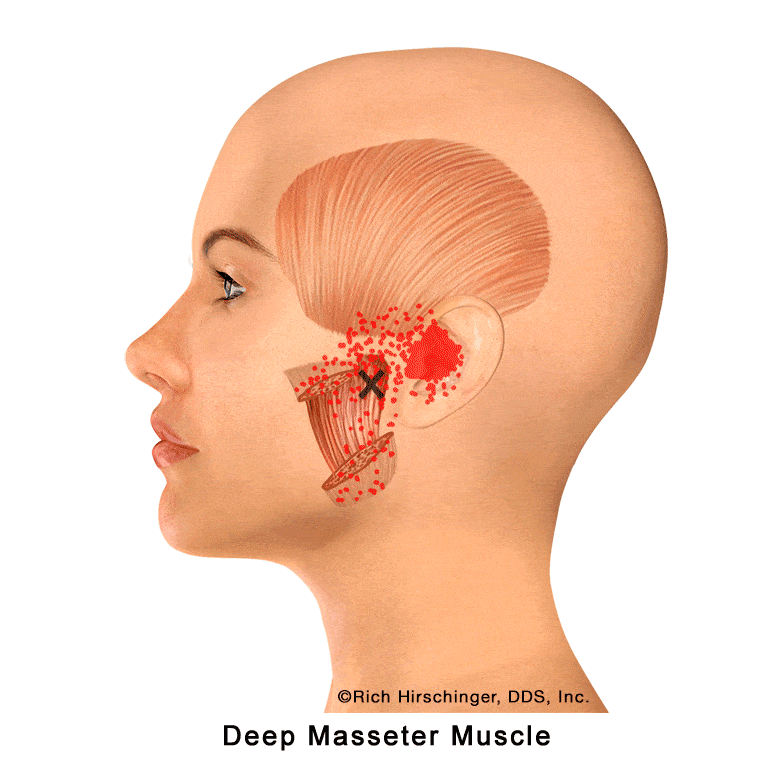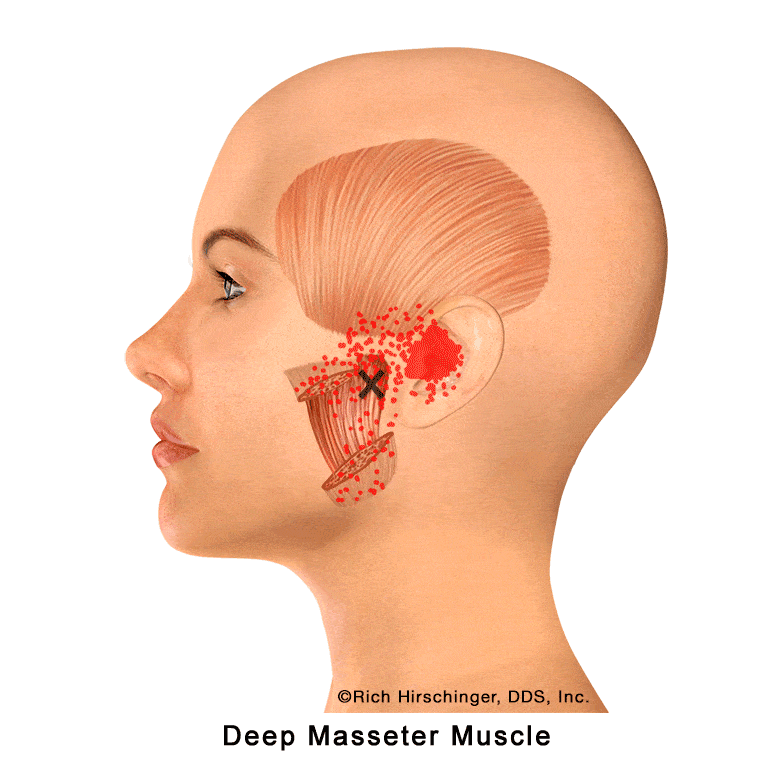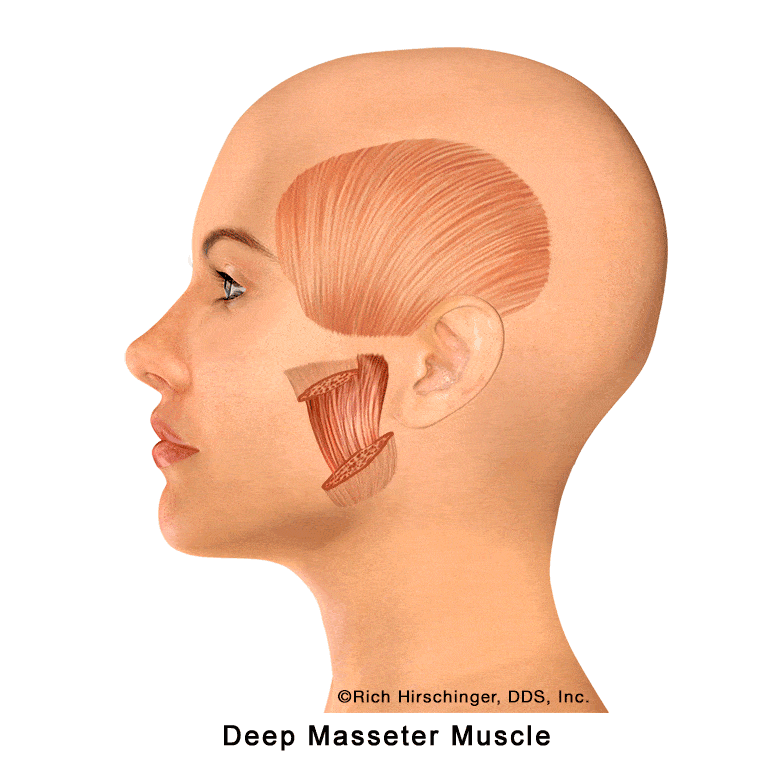
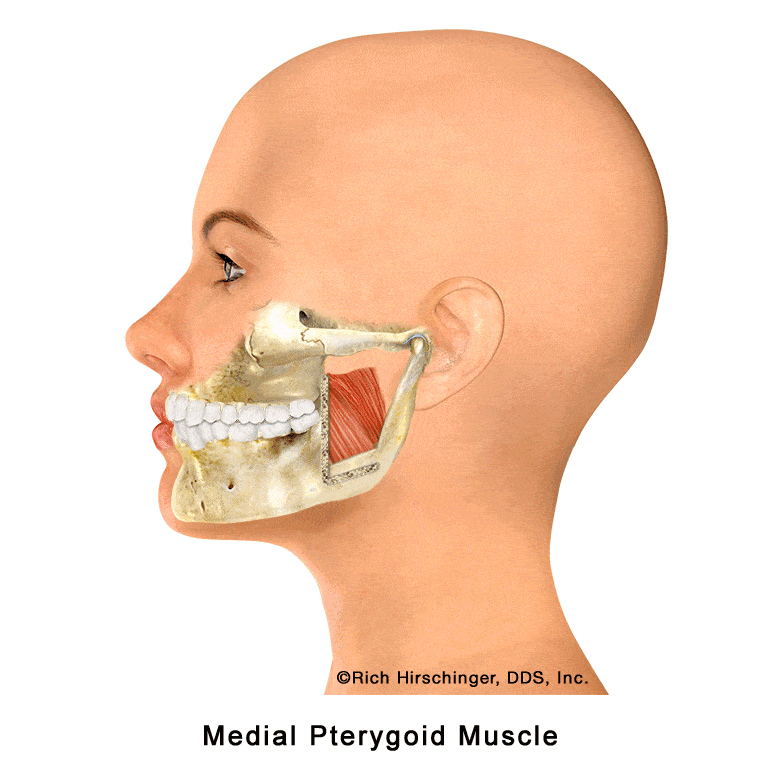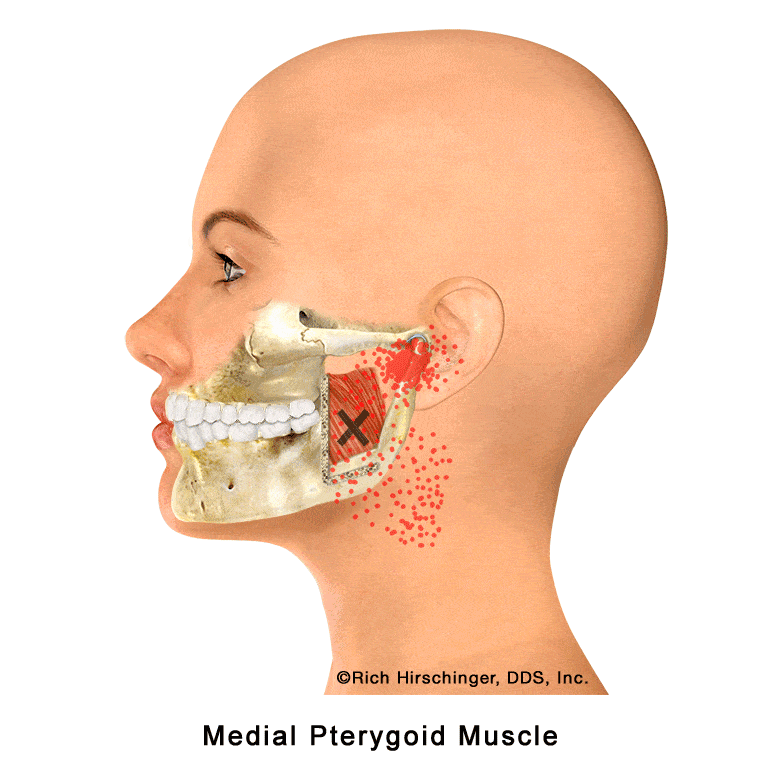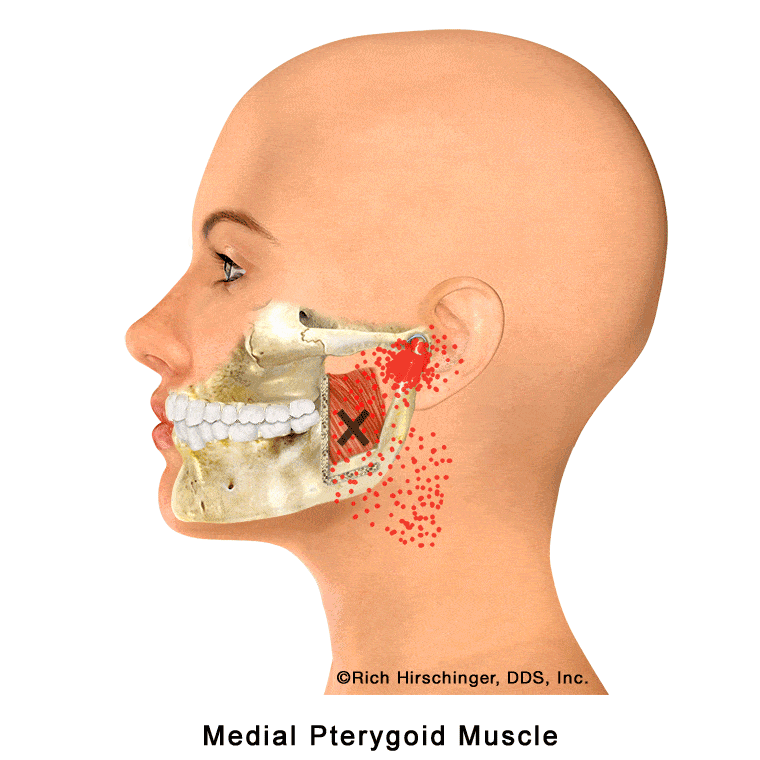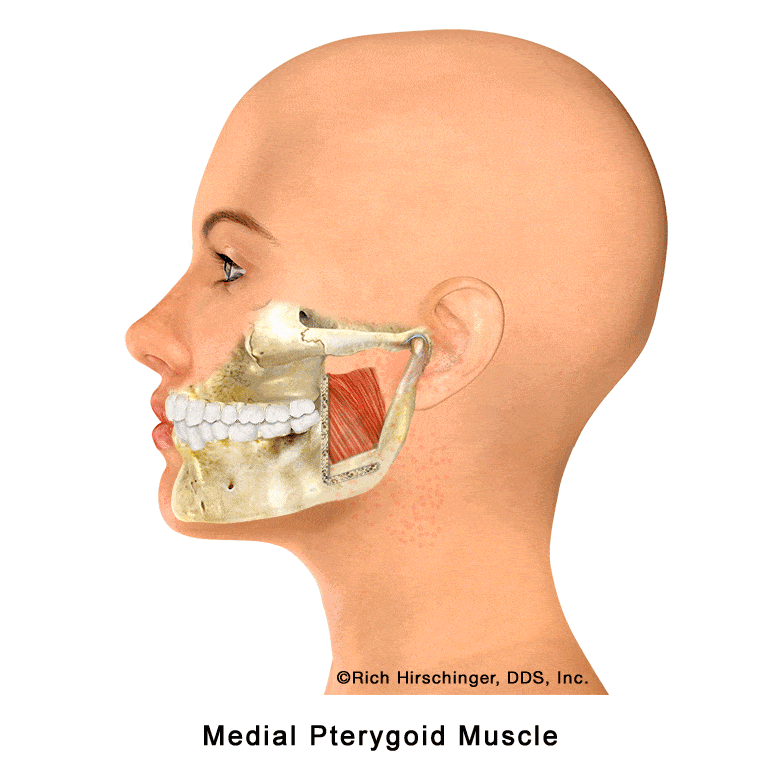
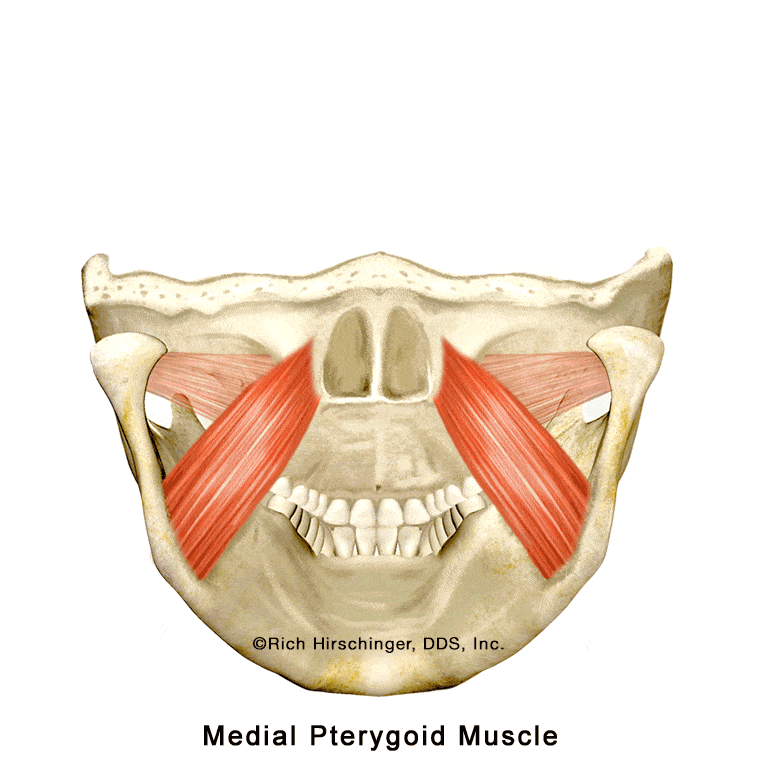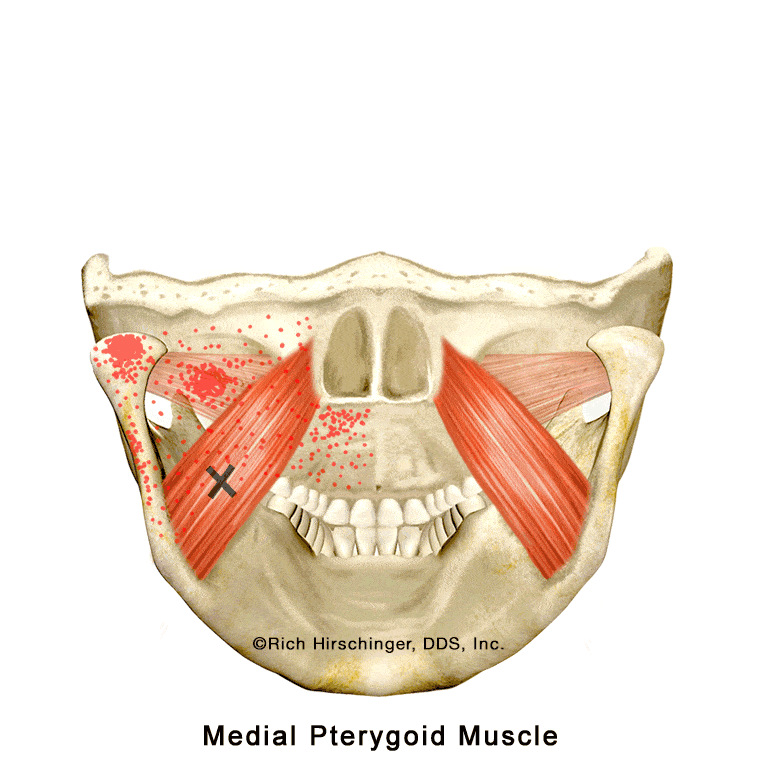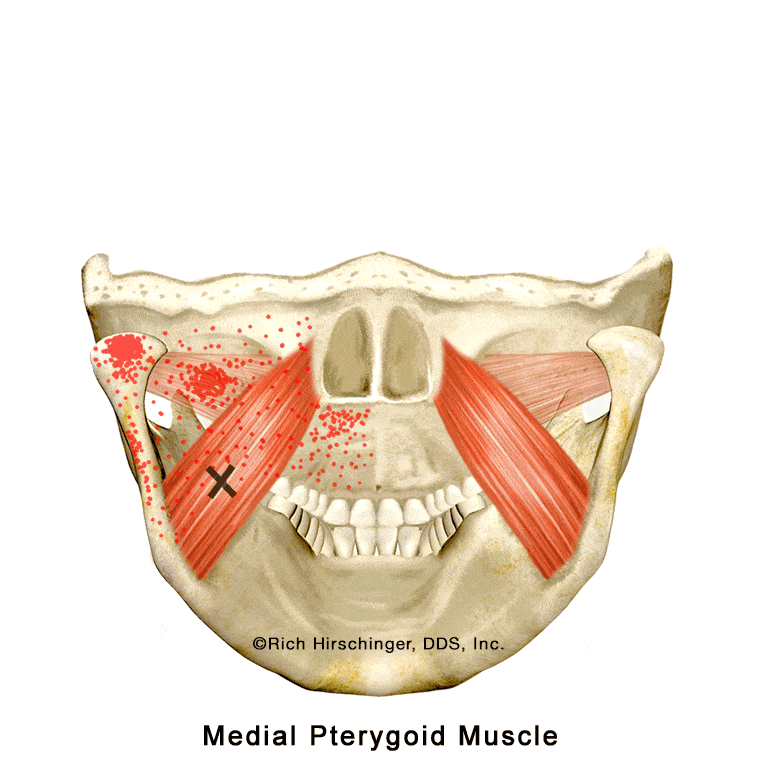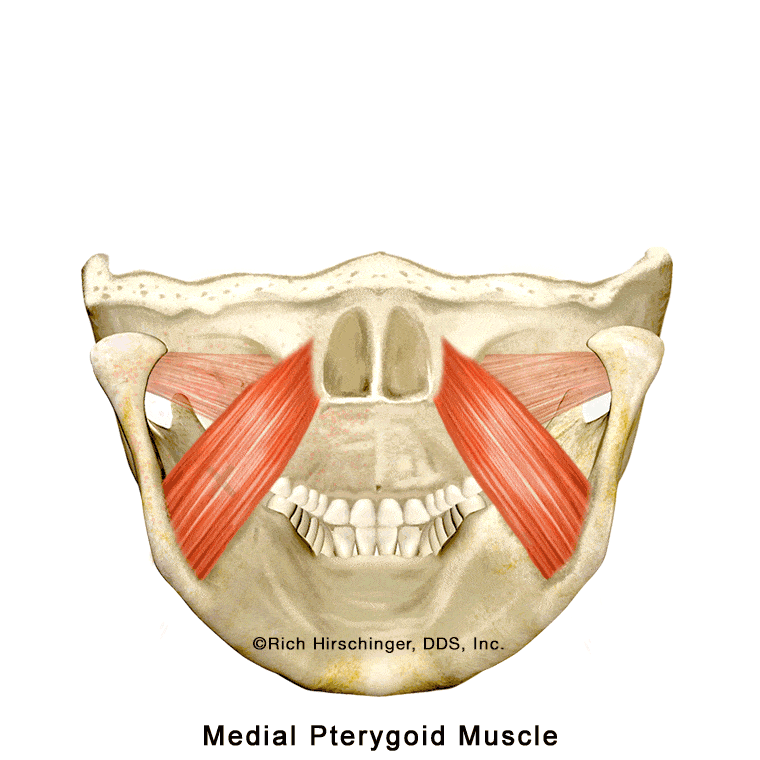
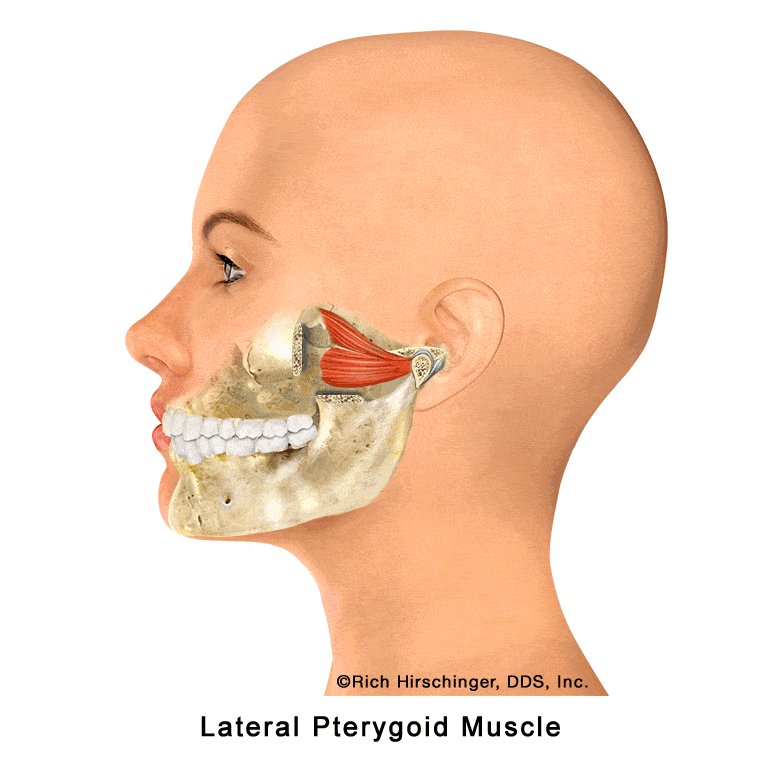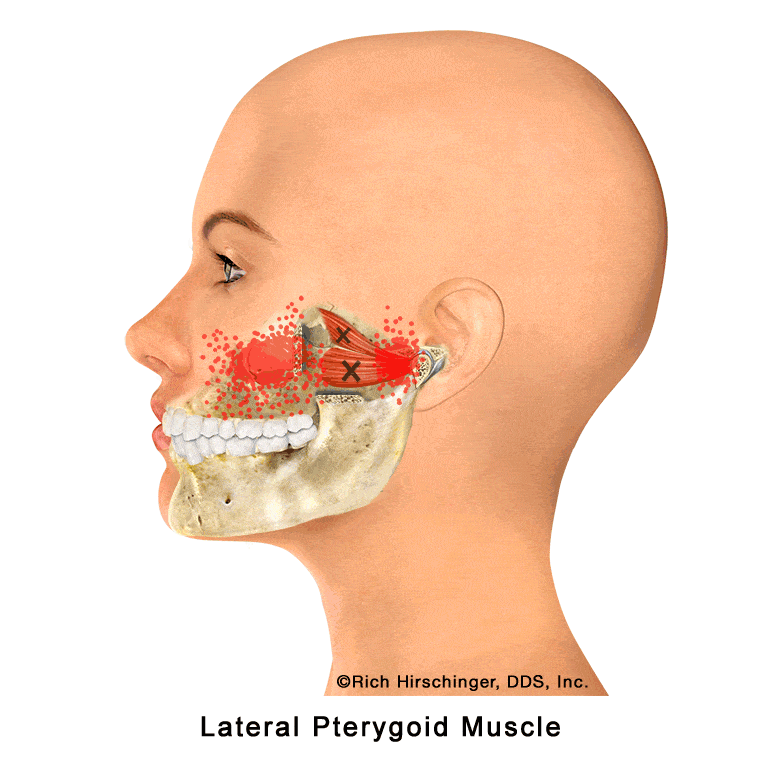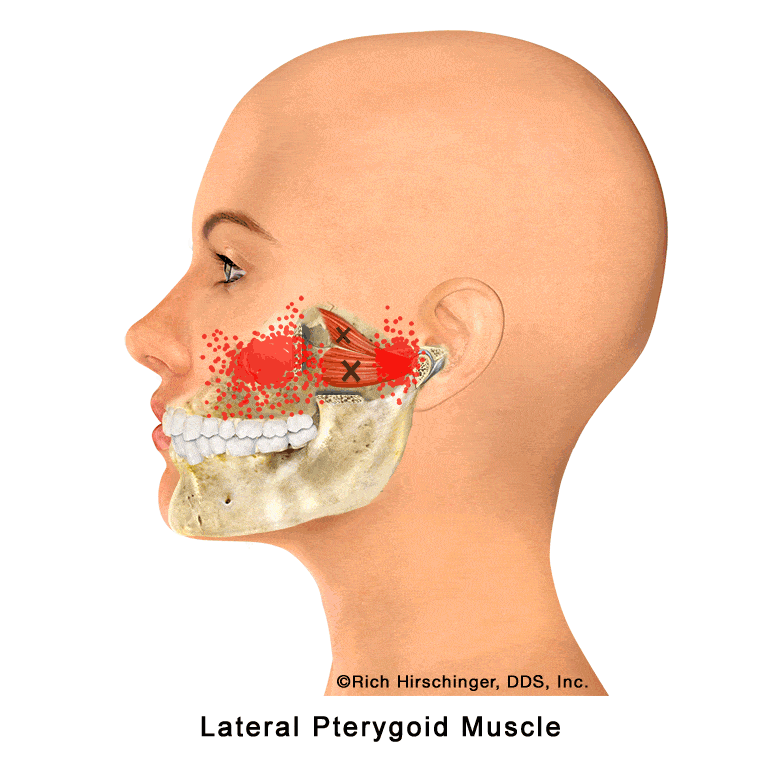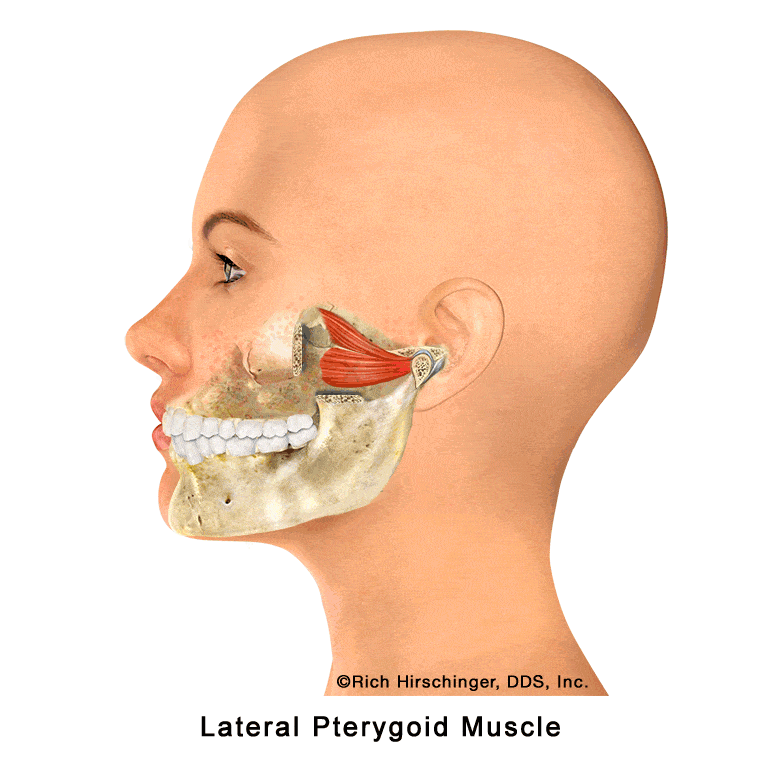
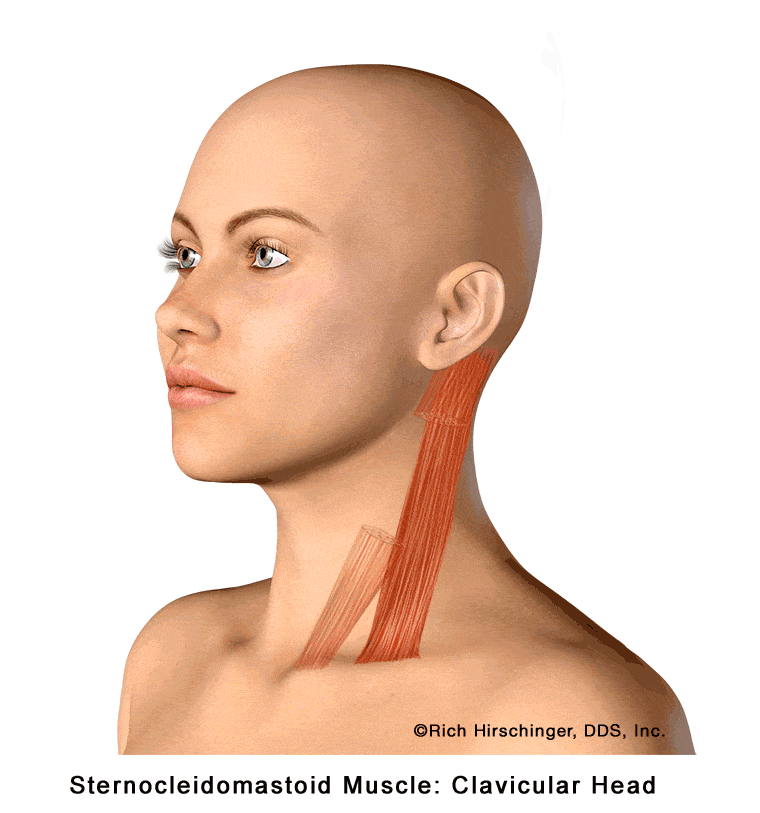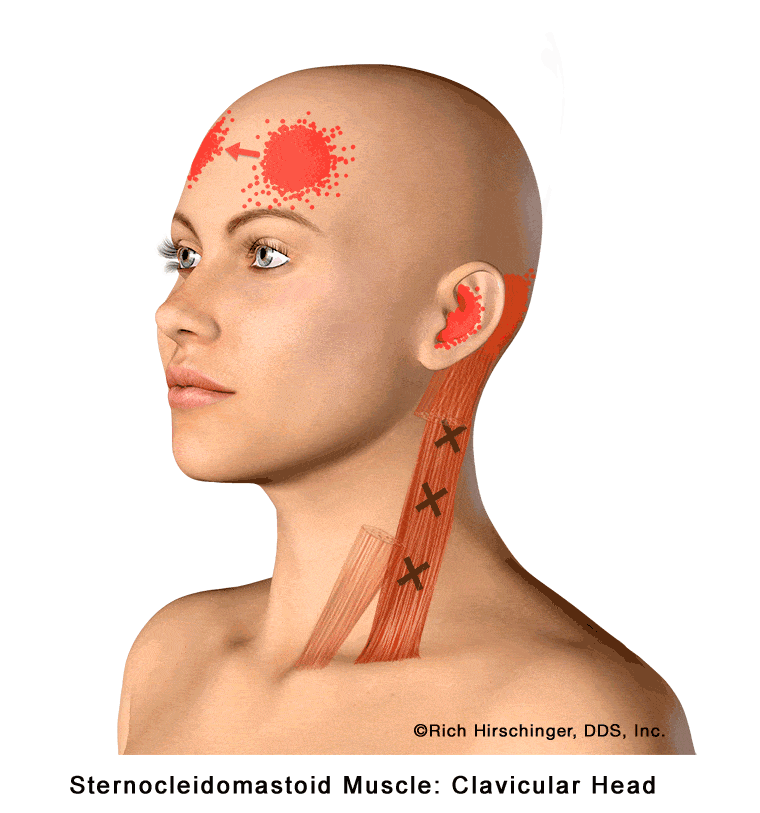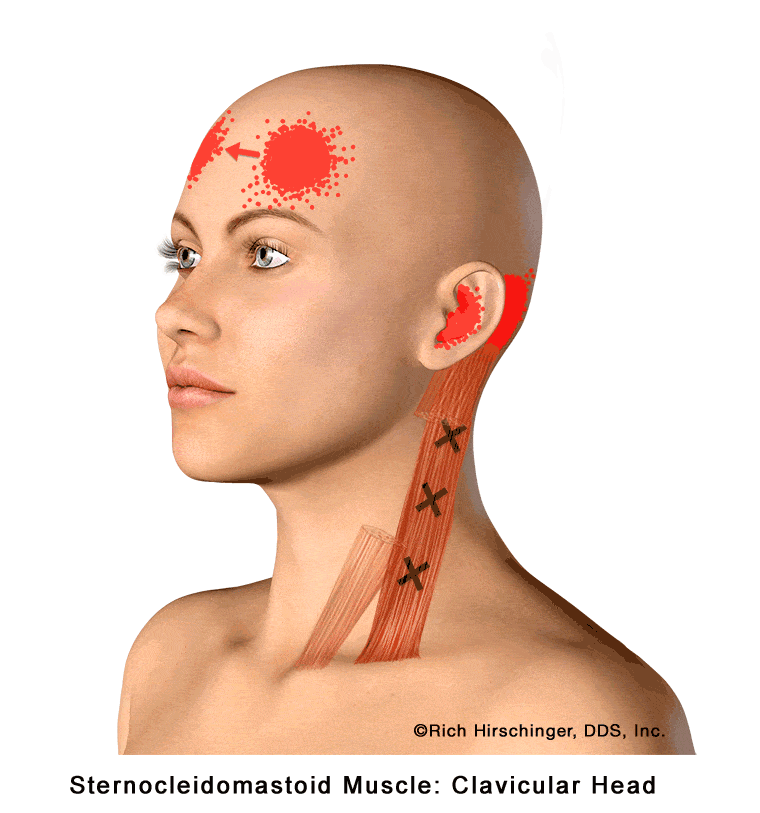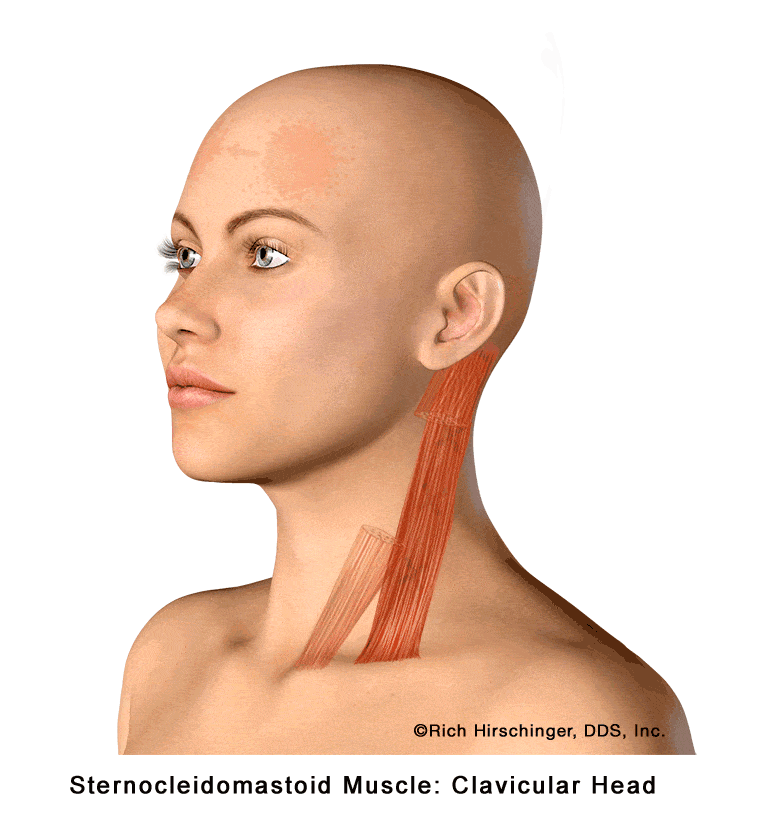
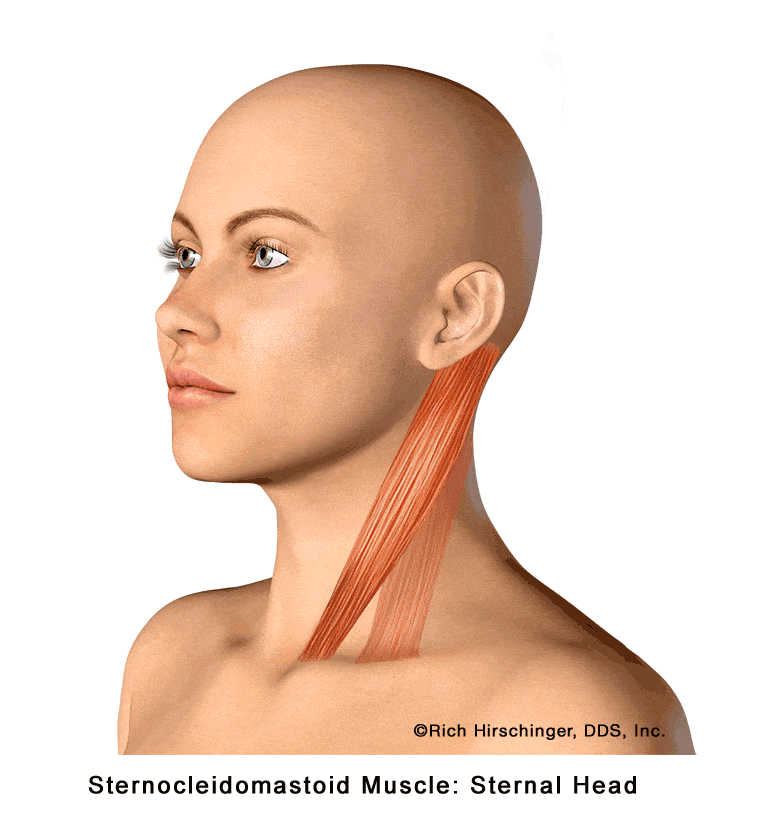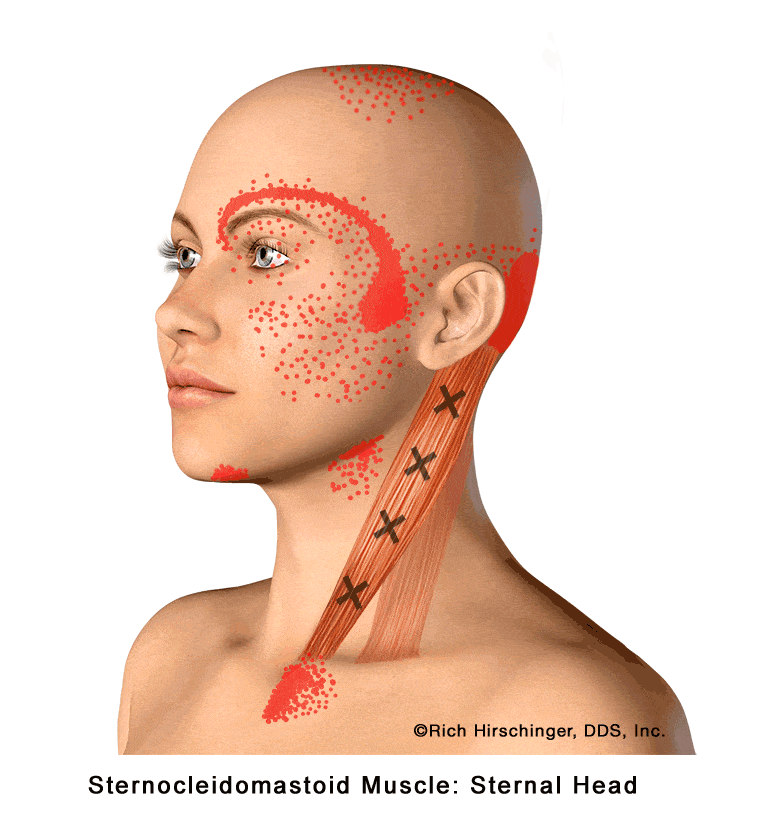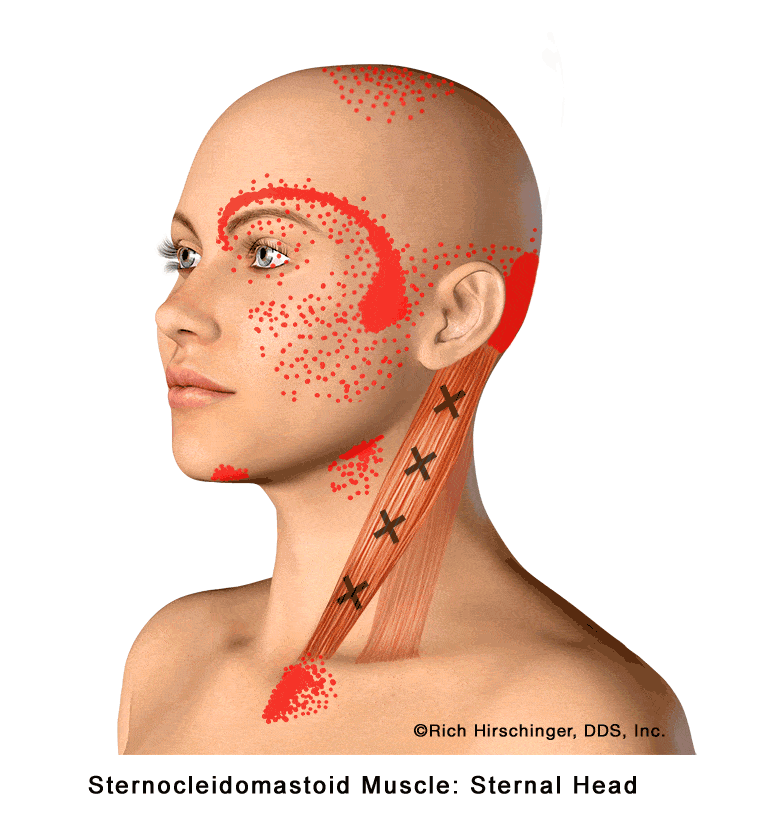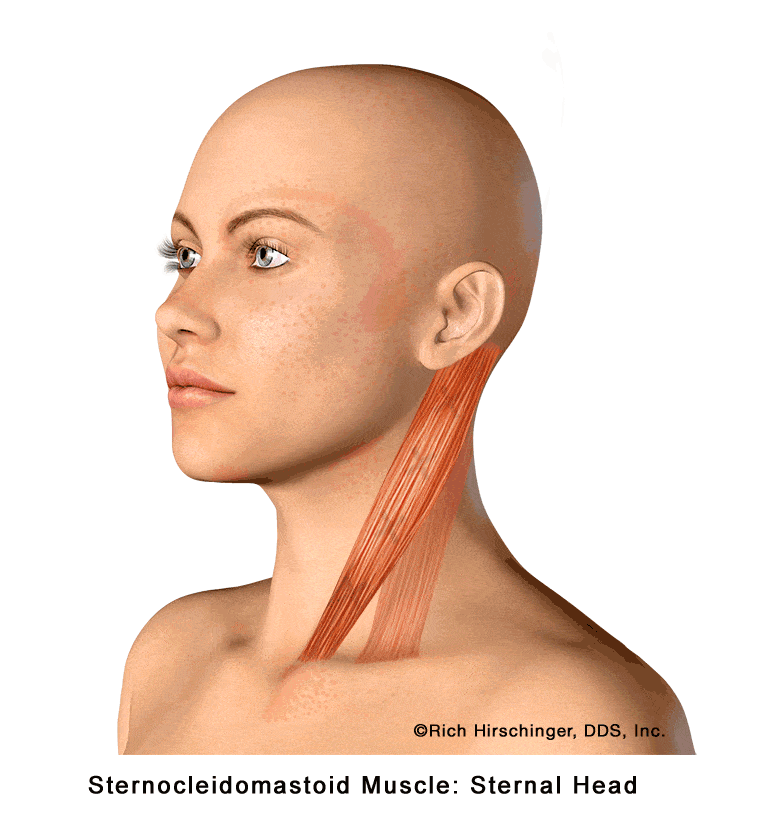
In the muscle referral pattern diagrams, the red areas indicate common sites of pain, whereas the black “X” marks the true muscular source of that pain. Darker red regions do not necessarily indicate more severe pain; rather, they indicate the most frequently reported locations of muscle-related jaw pain.
Recognizing that TMJ refers to an anatomical joint—not a diagnosis—helps patients and clinicians focus on identifying the true cause of jaw pain, which is often muscular and highly treatable with conservative care, such as the gentle jaw, a passive jaw-stretching device that Dr. Hirschinger invented.
Deep Masseter Muscle: A Key Jaw-Closing Muscle Beneath the Surface
The deep masseter is one of the four primary jaw-closing muscles involved in chewing, clenching, and stabilizing the jaw. It is located on the outer surface of the mandible (lower jaw), lying directly beneath the superficial masseter muscle.
Because of its deeper position, the deep masseter plays an important role in generating strong bite force and maintaining jaw stability during function. Overactivity from clenching, grinding (bruxism), or prolonged chewing can lead to muscle fatigue and tenderness, which may contribute to jaw pain and muscle-related “TMJ” symptoms.
Understanding the location and function of the deep masseter muscle is essential when evaluating patients with jaw muscle pain, facial soreness, or referred joint pain associated with temporomandibular disorders (TMD).
Medial Pterygoid Muscle: An Inside Jaw Muscle That Can Refer Pain
The medial pterygoid is one of the four primary jaw-closing muscles involved in chewing and clenching. (The “p” in pterygoid is silent.) This muscle is positioned on the inner side of the mandible (lower jaw), where it works together with the masseter and temporalis muscles to elevate and stabilize the jaw during biting and chewing.
In the animation, the highlighted red areas indicate locations where patients commonly report pain associated with medial pterygoid muscle tension or trigger points. A cutaway “window” in the jaw illustration shows how this muscle lies along the inside surface of the mandible, helping viewers understand why pain originating from this internal jaw muscle may be felt in nearby areas of the jaw, face, or throat.
Because the medial pterygoid is not visible externally, its role in jaw muscle pain and “TMJ” symptoms is often overlooked. Recognizing this muscle’s location and referral pain patterns is important when evaluating patients with jaw pain, clenching-related discomfort, or muscle-related temporomandibular disorders (TMD).
Lateral Pterygoid Muscle: Controls Side-to-Side and Forward Jaw Movement
The lateral pterygoid is one of the key muscles responsible for moving the jaw forward (protrusion) and side-to-side (lateral excursion). These movements are essential for normal chewing, speaking, and coordinated jaw function.
This muscle is highly active in patients who clench or grind their teeth (bruxism), which can cause it to become overworked, tight, and painful. When irritated, the lateral pterygoid may contribute to jaw pain, difficulty with smooth jaw movement, and symptoms often described as “TMJ pain,” even though the source of discomfort is muscular rather than joint-related.
Because the lateral pterygoid plays a major role in controlling jaw motion and stabilizing the temporomandibular joint during function, recognizing its involvement is important when evaluating muscle-related temporomandibular disorders (TMD) and bruxism-related jaw pain.
Clavicular Head of the Sternocleidomastoid (SCM) Muscle and Referred Pain Patterns
The clavicular head of the sternocleidomastoid muscle (SCM) is one of the primary muscles on the side of the neck responsible for lateral rotation and for assisting with neck flexion and stabilization. This muscle plays an important role in everyday movements, including looking over the shoulder, tilting the head, and maintaining head posture.
When the clavicular head of the SCM becomes tight, strained, or develops trigger points—often due to poor posture, stress, or prolonged head-forward positioning—it can produce referred pain in several characteristic areas. Patients may experience pain in or around the ear, behind the ear (mastoid region), across the forehead, and even in the opposite side of the forehead.
Because these referral patterns can mimic ear disorders, sinus problems, or headache conditions, recognizing SCM-related referred pain is essential when evaluating patients with head, neck, and facial pain that does not originate from the ear or teeth.
Sternal Head of the Sternocleidomastoid (SCM) Muscle and Its Referred Pain Patterns
The sternal head of the sternocleidomastoid muscle (SCM) is the more superficial portion of this prominent neck muscle located along the side of the neck. It plays a key role in turning the head side to side, flexing the neck, and helping maintain head and neck posture during daily activities.
When the sternal head of the SCM becomes tight, strained, or develops myofascial trigger points—often due to poor posture, stress, or prolonged head-forward positioning—it can produce a wide range of referred pain symptoms. Common referral areas include pain in front of the ear, behind the ear, across the forehead, into the cheek, chin, and eye, as well as under the jaw and even into the upper chest or breastbone (sternal) region.
Because these referral patterns can mimic ear disorders, sinus pain, facial pain, dental pain, or temporomandibular disorder (TMD) symptoms, recognizing SCM muscle involvement is essential when evaluating patients with head, neck, and facial pain without a clear dental or ear-related cause.
Learn about referred muscle pain into teeth.
Learn about appliances for TMJ.
Learn about Botox for TMJ and jaw muscle pain.
All images are the copyright of Rich Hirschinger, DDS, Inc., and were created under the direction of Dr. Hirschinger. The unedited images can be used with permission by completing the form on this page on the gentle jaw website. All rights reserved.
