Jaw Closing Muscles That Refer Pain Into Teeth
Why Jaw Muscle Pain Can Feel Like a Toothache
Many patients are surprised to learn that pain felt in a tooth is not always caused by the tooth itself. In many cases, the true source of pain is a jaw-closing muscle. This phenomenon is known as referred pain, meaning that the pain is felt in a location different from where it originates.
Myofascial trigger points in the chewing muscles can mimic dental pain so closely that patients may believe they need a root canal or other dental treatment, even when the teeth are healthy.
Understanding these muscle referral patterns is essential when evaluating patients with persistent tooth pain that cannot be explained by dental disease.
The Jaw-Closing Muscles That Commonly Refer Pain to Teeth
Two of the muscles that close the jaw are the superficial masseter and temporalis muscles. When these muscles become overworked from clenching, grinding, stress, or prolonged jaw use, they can develop sensitive trigger points that refer pain into specific teeth.
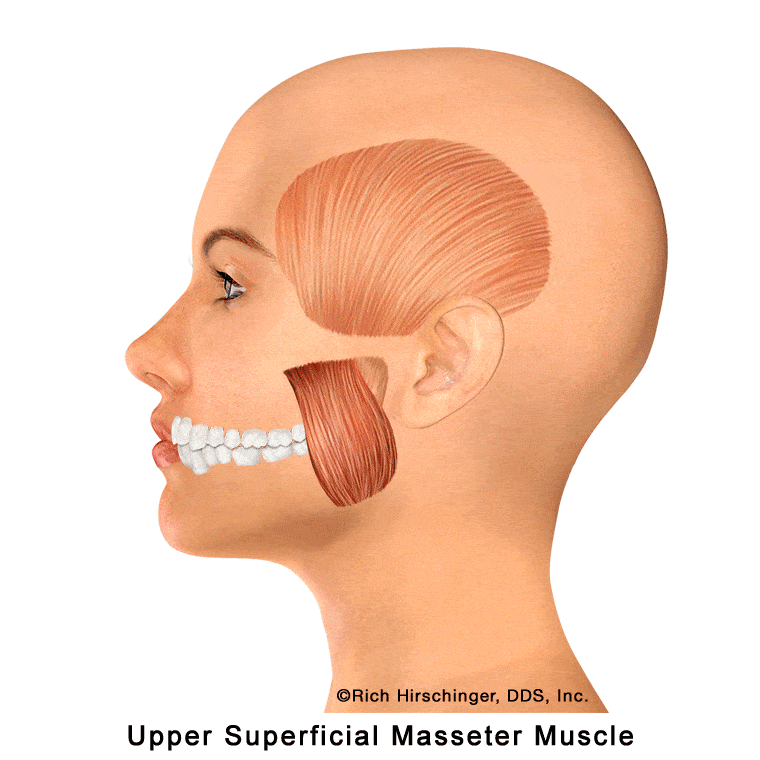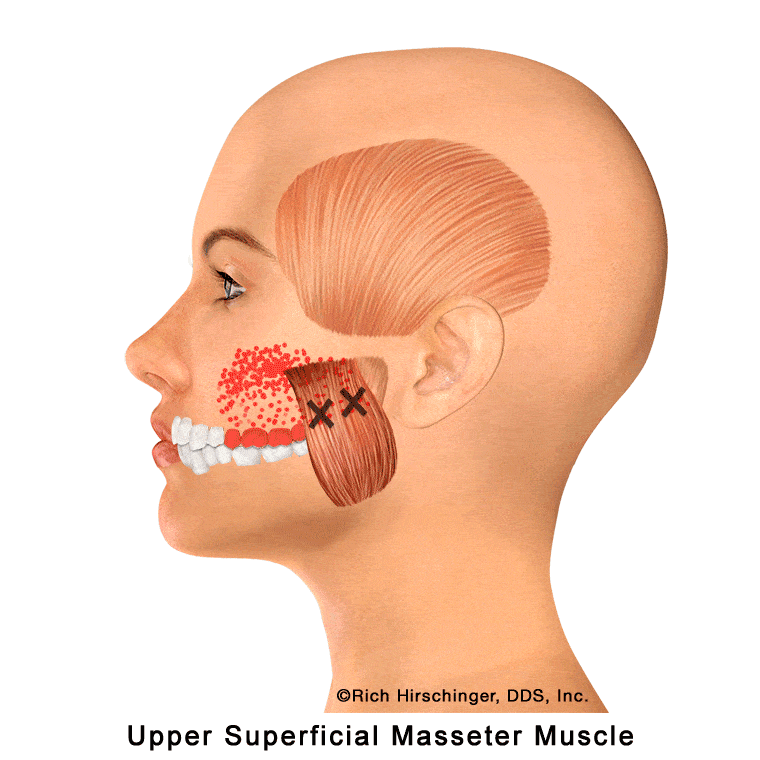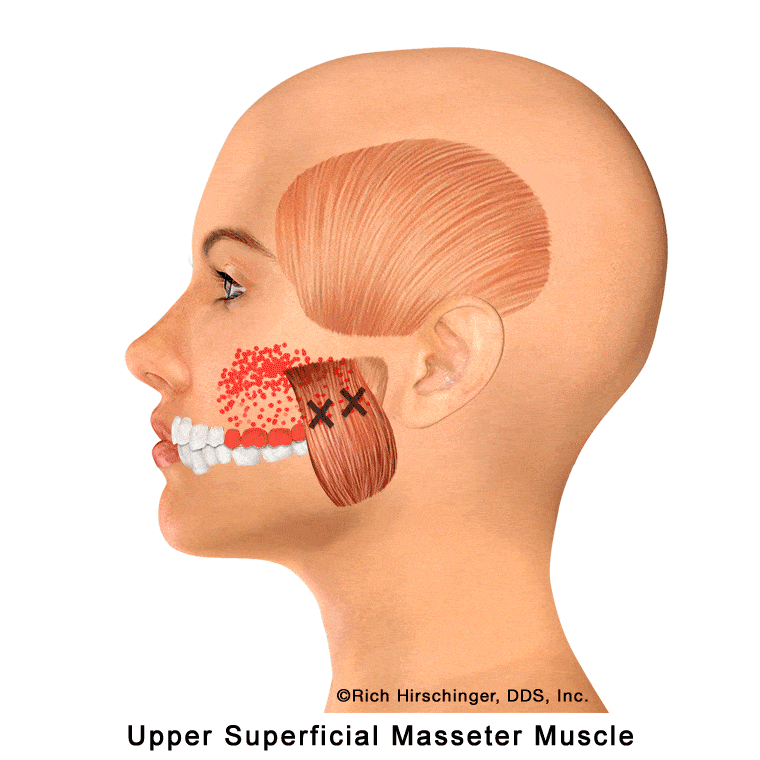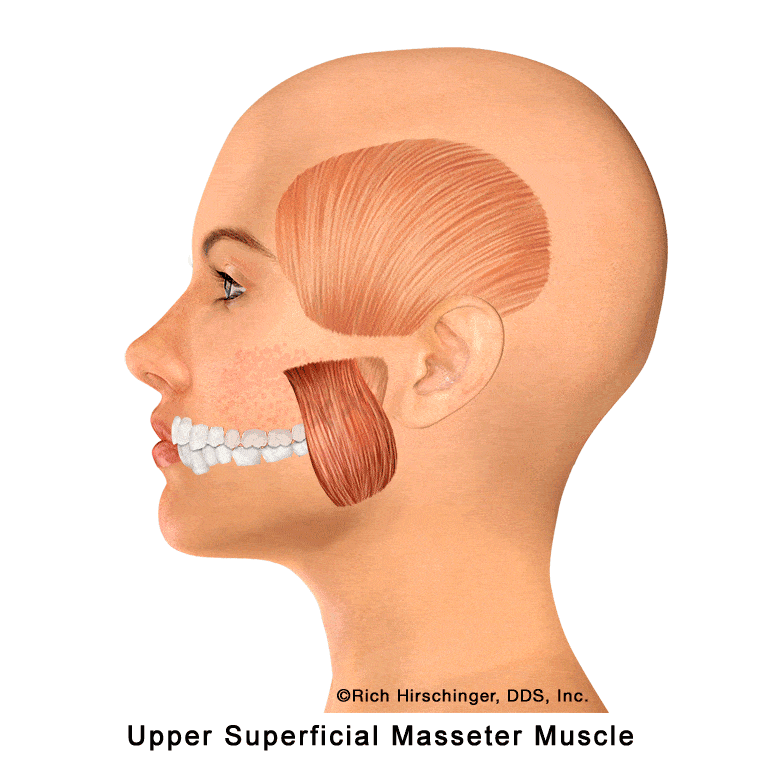
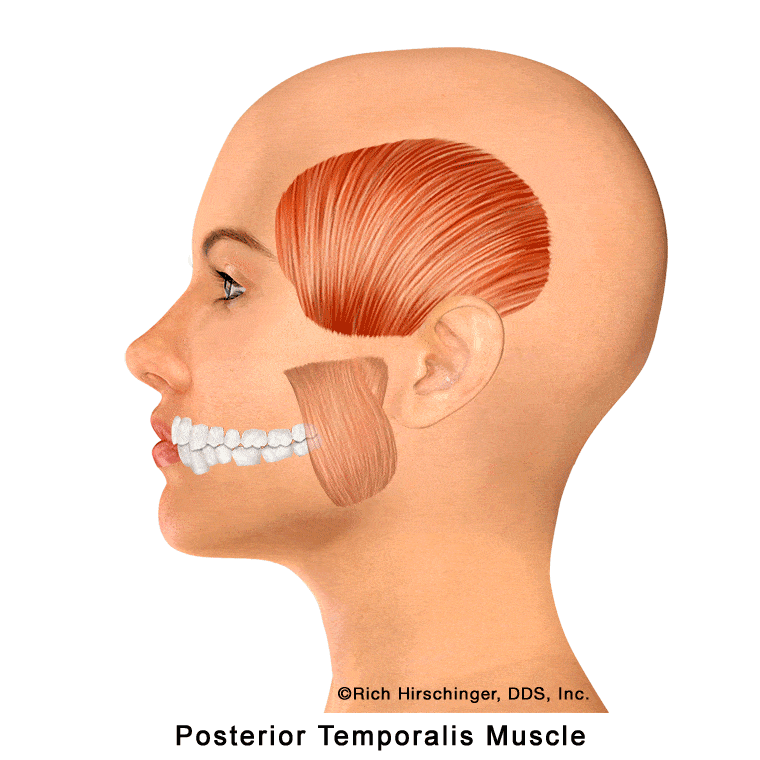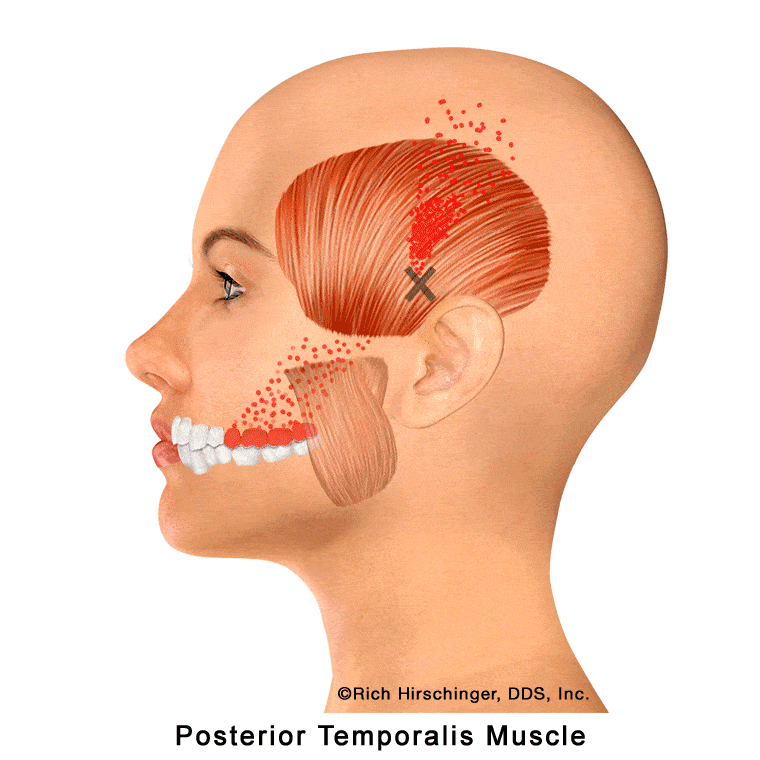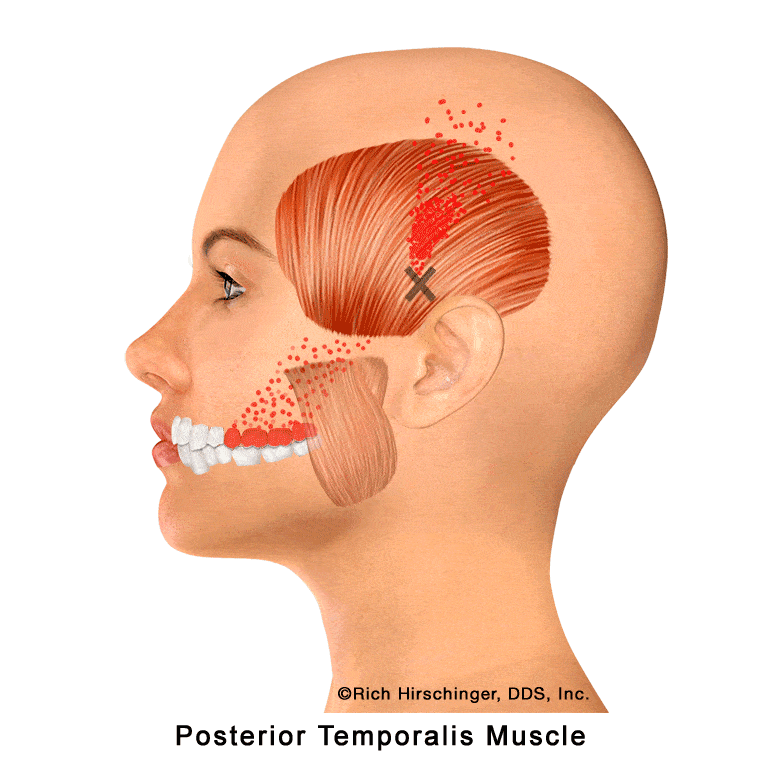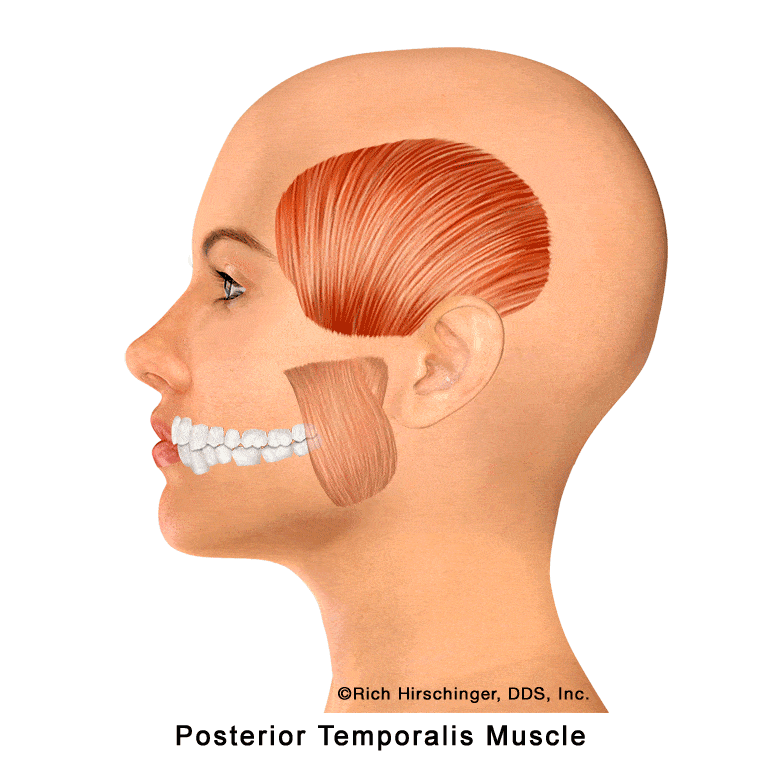
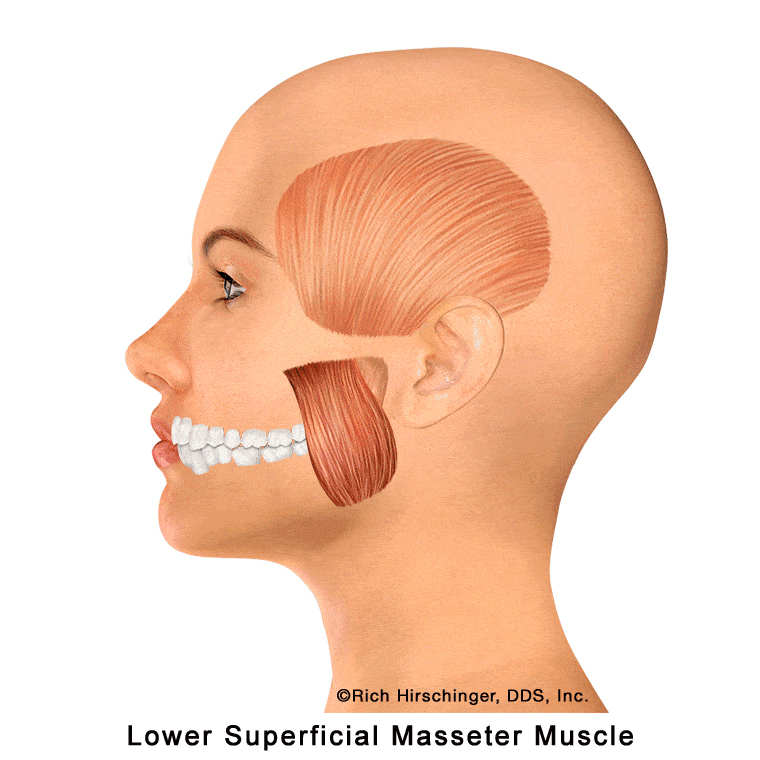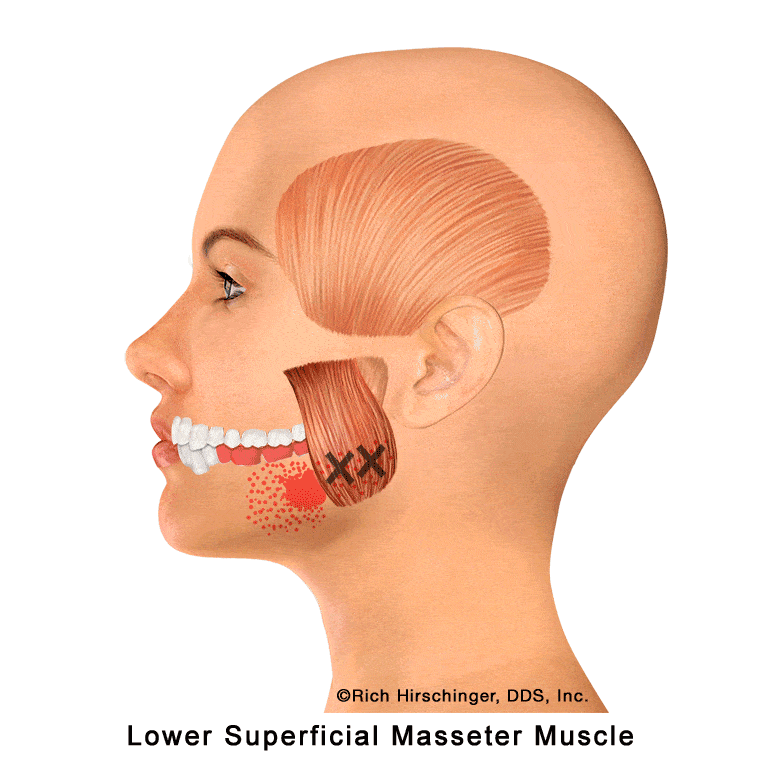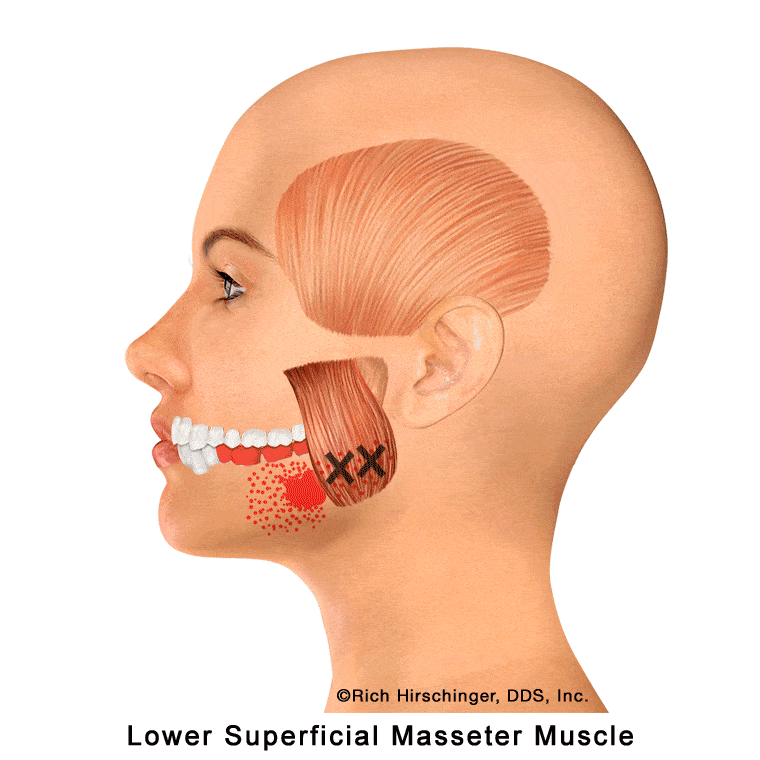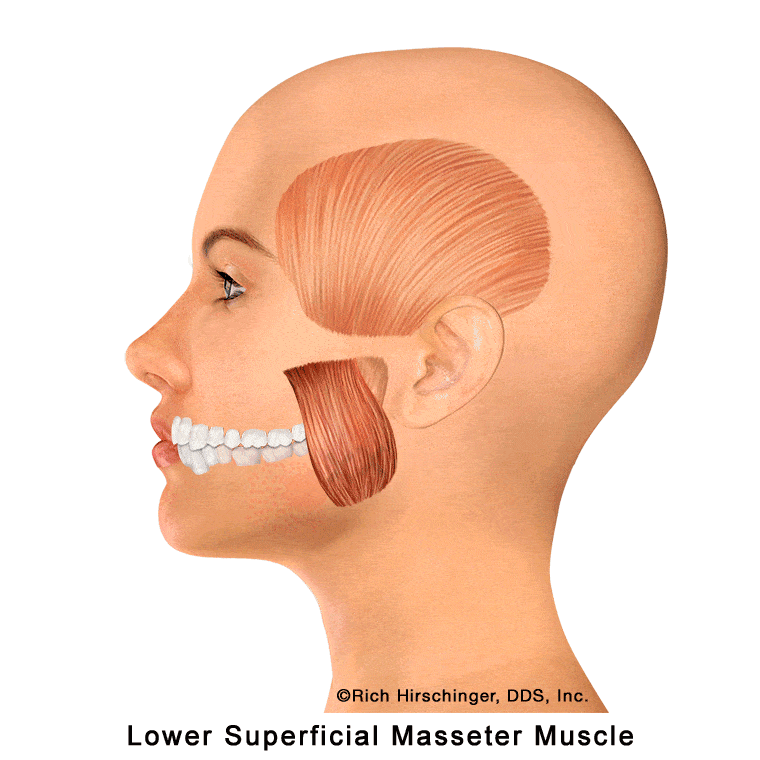
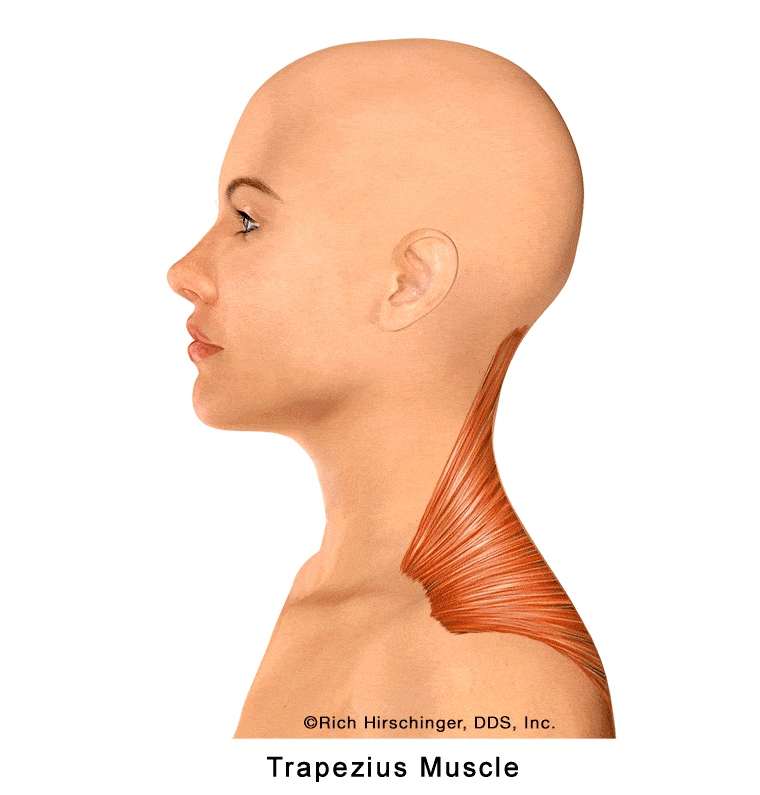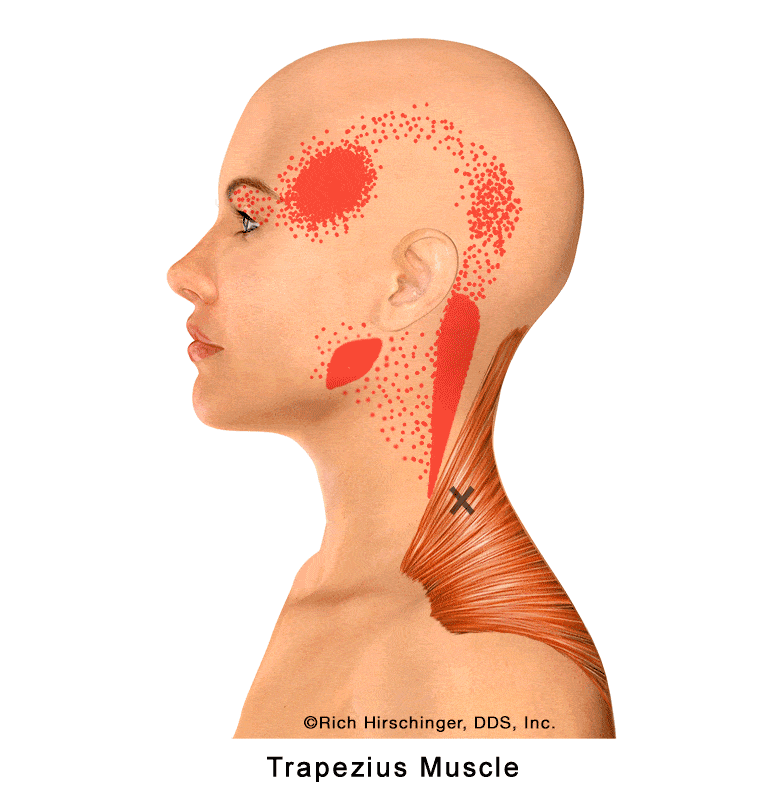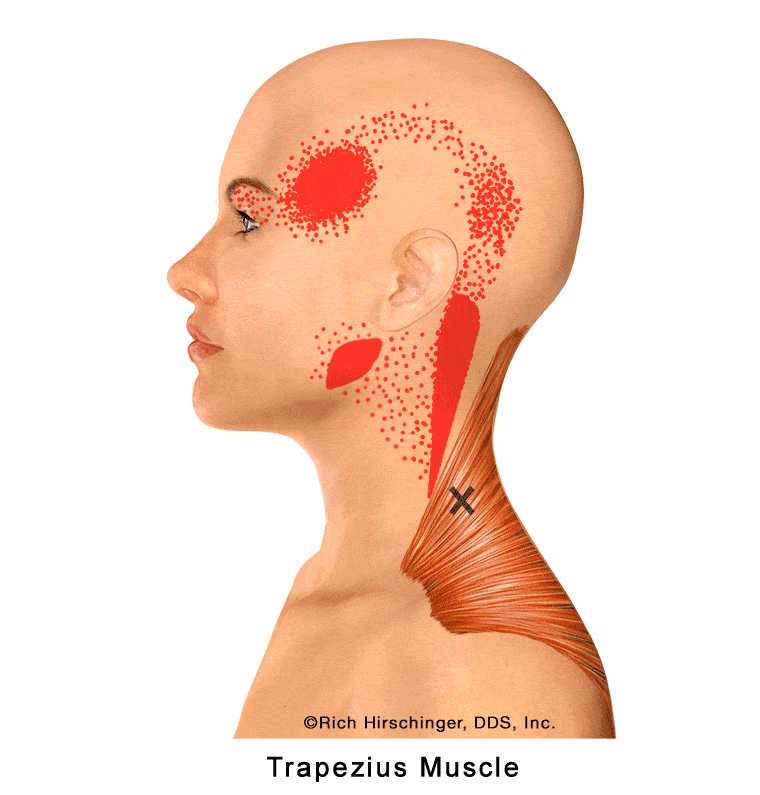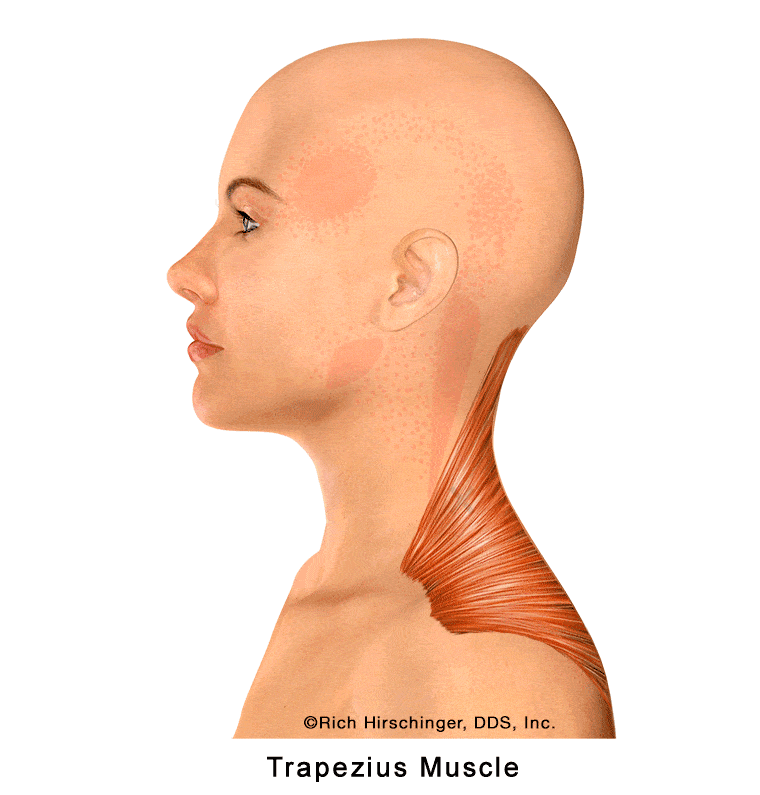
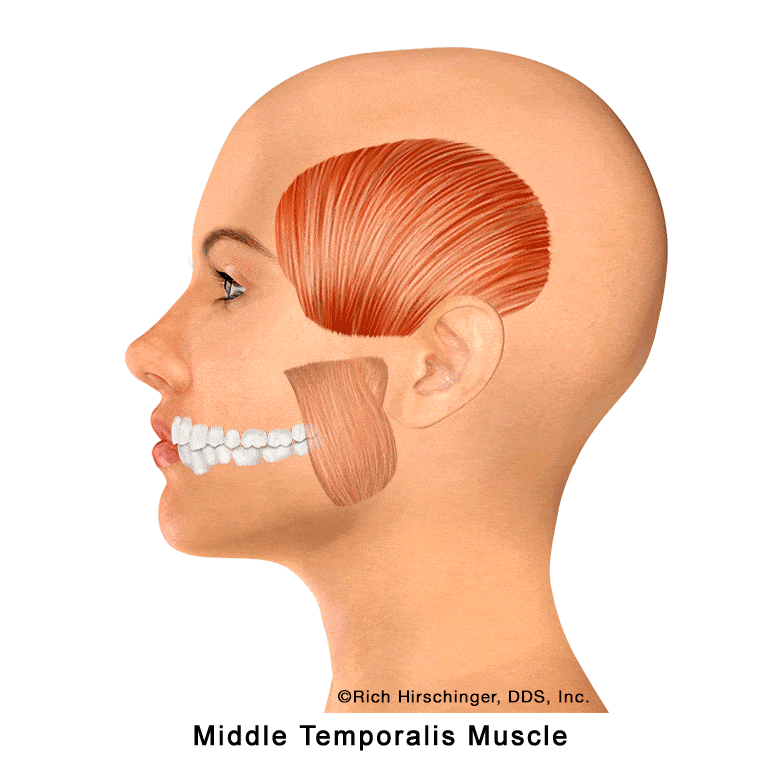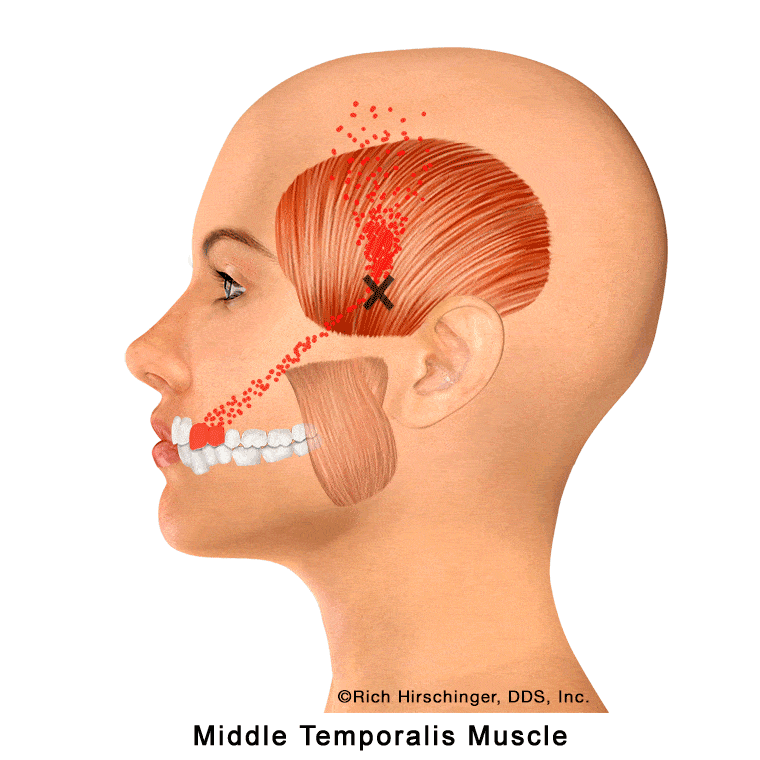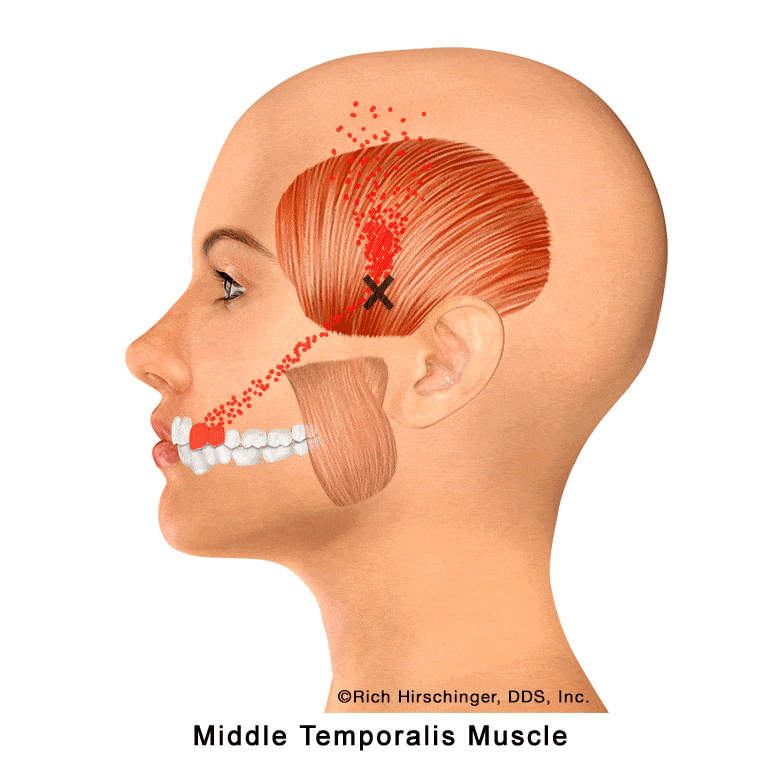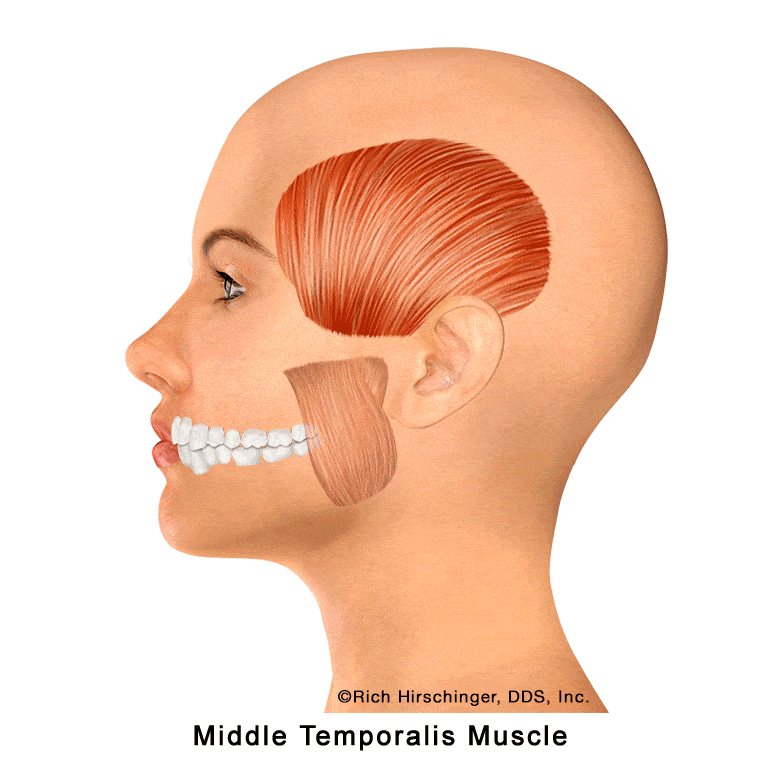
In the muscle referral pattern diagrams, the red areas indicate common sites of pain, whereas the black “X” marks the true muscular source of that pain. Darker red regions do not necessarily indicate more severe pain; rather, they indicate the most frequently reported locations of muscle-related jaw pain.
Upper Superficial Masseter Muscle: Referred Pain to Maxillary Teeth and Cheek/Sinus Region
The upper portion of the superficial masseter muscle is one of the primary jaw-closing muscles involved in chewing and clenching. When this muscle becomes overactive or develops myofascial trigger points—often due to clenching, grinding (bruxism), stress, or prolonged jaw use—it can refer pain into specific areas of the face and upper teeth.
Common referral patterns from the upper superficial masseter include pain in the maxillary molars and second premolar, as well as in the cheek and sinus regions. Because these symptoms can closely mimic a toothache or sinus-related pain, the true muscular source is often overlooked.
Recognizing this referral pattern is important when evaluating patients with upper back tooth pain or cheek discomfort that persists despite normal dental and sinus findings, as the origin may be muscle-related rather than odontogenic or sinus in nature.
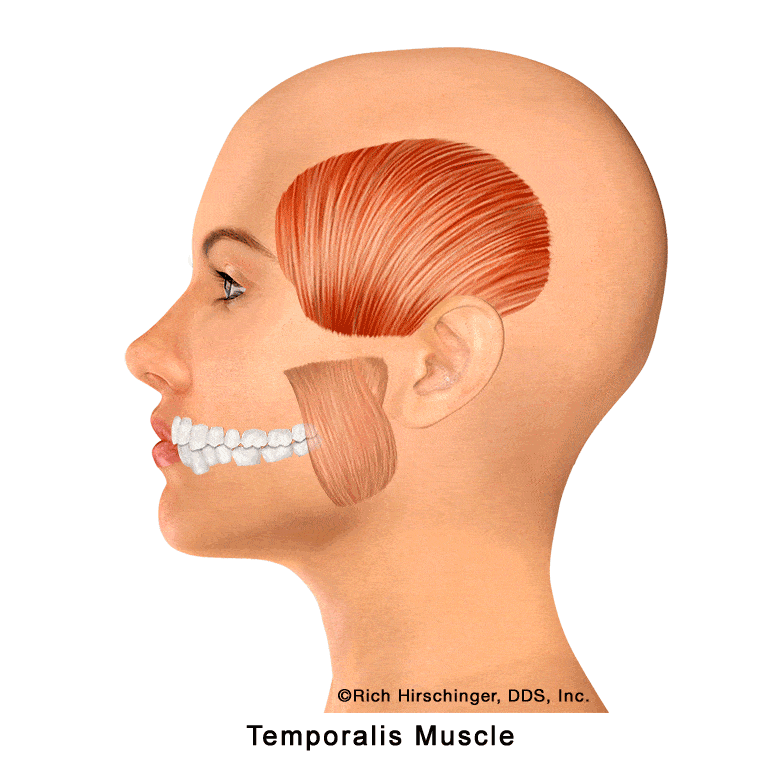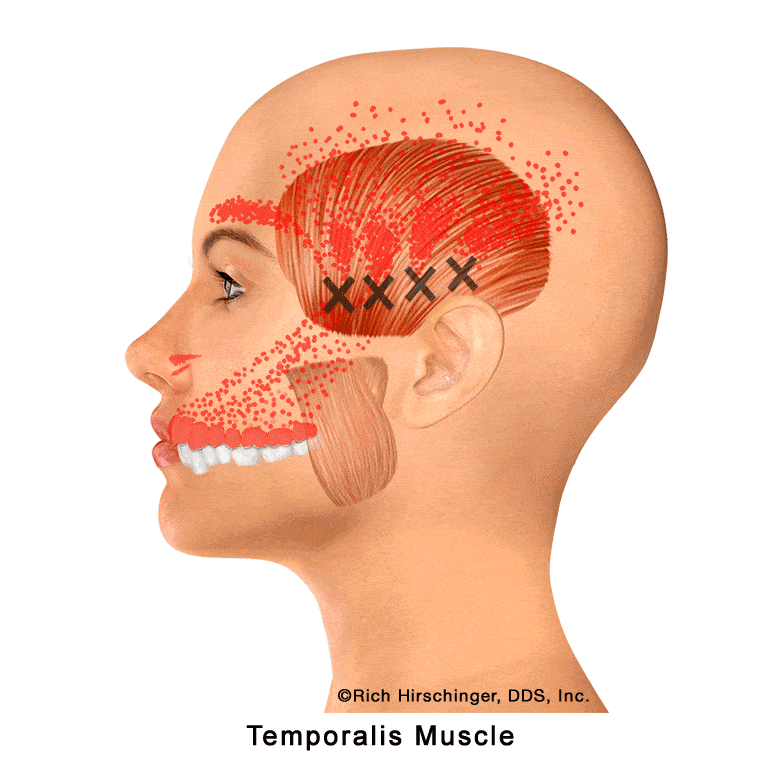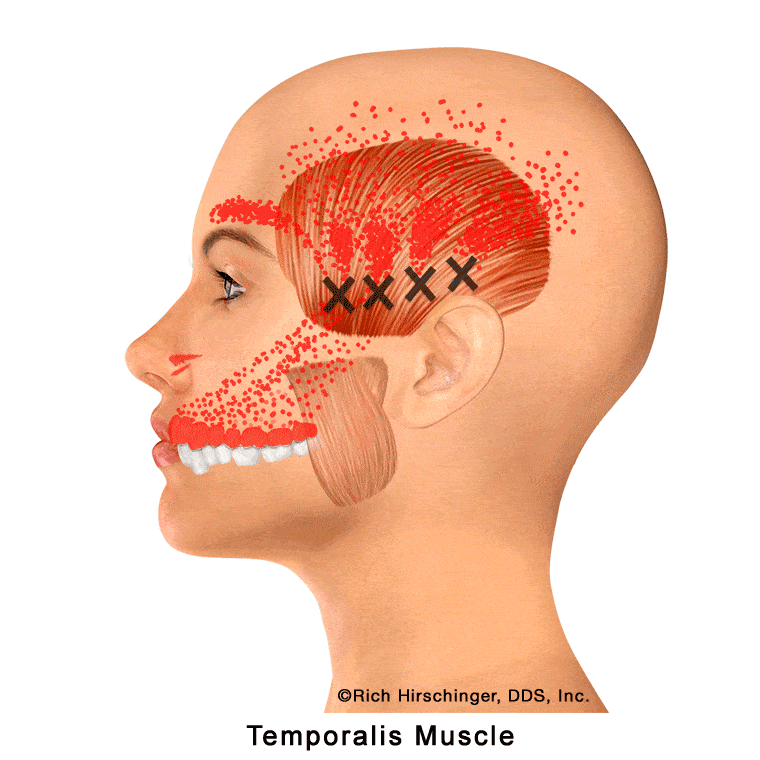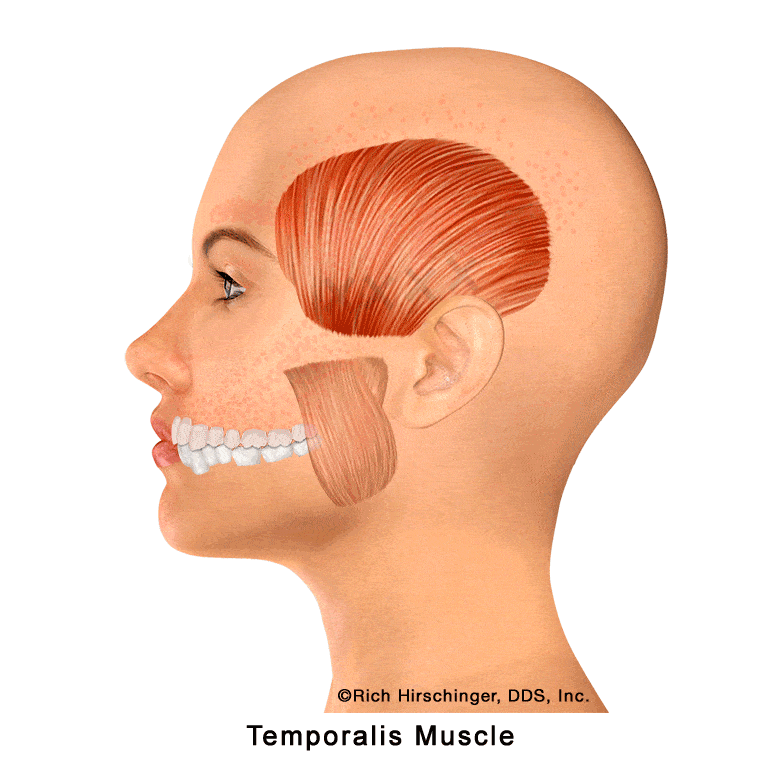
Posterior Temporalis Muscle: Referred Pain to Upper Molars, Second Premolar, Cheek/Sinus Area, and Temple
The posterior portion of the temporalis muscle is one of the key jaw-closing muscles that assists with elevating and retracting the mandible during chewing and clenching. Located at the back of the temple region, this muscle is frequently involved in muscle-related jaw pain and temporomandibular disorders (TMD).
When the posterior temporalis develops myofascial trigger points—often due to clenching, grinding (bruxism), or prolonged jaw tension—it can refer pain to several characteristic locations. Common referral areas include the maxillary molars, the second premolar, the cheek and sinus region, and the posterior temple area.
Because these referral patterns can closely mimic toothache or sinus-related pain, patients may mistakenly believe they have a dental or sinus problem when the true source is muscular. Recognizing posterior temporalis referral patterns is essential when evaluating persistent upper back tooth pain, temple headaches, or cheek discomfort that is not explained by dental or sinus disease.
Lower Superficial Masseter Muscle: Referred Pain to the Mandibular Molars, Second Premolar, and Jaw
The lower portion of the superficial masseter muscle is a primary jaw-closing muscle that plays a major role in chewing and clenching. When this muscle becomes overworked or develops myofascial trigger points—commonly due to clenching, grinding (bruxism), gum chewing, or prolonged jaw tension—it can produce referred pain to the mandibular (lower) molars and the jaw.
This type of muscle-related referred pain can closely resemble a true toothache, even when the teeth themselves are healthy. Patients may report aching, pressure, or sensitivity in the lower back teeth without clear dental findings. Recognizing the lower superficial masseter as a potential source of mandibular molar pain is important when evaluating jaw muscle pain and temporomandibular disorders (TMD), helping to prevent unnecessary dental treatment and focus on appropriate muscle-based care.
Trapezius Muscle: A Shoulder Muscle That Can Refer Pain to the Angle of the Jaw, Eyes, Temples, etc.
The trapezius muscle is a large shoulder and upper back muscle that supports head posture, elevates the shoulders, and stabilizes the neck and upper spine. Although it is not a jaw-closing muscle, it can still play an important role in head, neck, and jaw pain since it can and does refer pain into the jaw.
Trigger points in the upper trapezius can refer pain to the angle of the mandible (lower jaw), creating symptoms that may be mistaken for jaw muscle pain or “TMJ” discomfort. Patients may describe aching or soreness near the jawline that worsens with stress, poor posture, prolonged computer use, or neck strain.
Because trapezius-related referred pain can mimic true jaw muscle pain, the trapezius should be carefully evaluated and excluded as a contributing source when patients present with persistent lower jaw pain, facial discomfort, or muscle-related temporomandibular disorder (TMD) symptoms.
Anterior Temporalis Muscle: Referred Pain to the Maxillary Anterior Teeth, Nose, Above the Eye, etc.
The anterior portion of the temporalis muscle is one of the primary jaw-closing muscles responsible for elevating the mandible during biting and chewing. Located in the anterior region of the temple, this muscle is frequently implicated in clenching-related jaw muscle pain and temporomandibular disorders (TMD).
When the anterior temporalis develops myofascial trigger points—often due to clenching, grinding (bruxism), stress, or prolonged jaw tension—it can refer pain to the maxillary (upper) anterior teeth, the side of the nose, above the eye, and the temple. Patients may experience aching, pressure, or sensitivity in the upper front teeth even when the teeth themselves are healthy and show no signs of dental disease.
Because this referral pattern can closely mimic true dental pain, recognizing the anterior temporalis muscle as a potential source is important when evaluating unexplained upper anterior tooth discomfort, particularly in patients with jaw muscle tension or daytime clenching.

Middle Temporalis Muscle: Referred Pain to Maxillary Canines, Premolars, Temple, and Cheek/Sinus Area
The middle portion of the temporalis muscle is an important jaw-closing muscle that elevates the mandible during chewing and clenching. Located in the central temple region, this muscle is commonly involved in temporomandibular disorders (TMD) and in clenching or grinding (bruxism) habits.
When the middle temporalis develops myofascial trigger points—often due to stress, jaw overuse, or prolonged clenching—it can produce characteristic referred pain patterns. These commonly include pain in the maxillary (upper) canines and first premolar, discomfort over the temple, and a small area of the cheek and sinus region.
Because these referral patterns can mimic dental pain or sinus-related symptoms, identifying involvement of the middle temporalis muscle is essential when evaluating patients with unexplained upper canine or premolar pain, temple headaches, or cheek/sinus discomfort that is not due to primary dental or sinus disease.
Combined Temporalis Muscle Referral Patterns: Pain in Upper Teeth, Temple, Cheek, Nose, and Above the Eye
When the referral patterns of all portions of the temporalis muscle (anterior, middle, and posterior fibers) are considered together, it becomes clear that this single jaw-closing muscle can refer pain to a wide range of areas in the face and head.
Collectively, temporalis muscle trigger points can produce referred pain affecting all of the maxillary (upper) teeth, the entire temple region, the cheek, the side of the nose, and the area above the eye. Because of this broad distribution, temporalis-related myofascial pain is frequently mistaken for dental pain, sinus discomfort, or headache disorders.
Understanding these combined referral patterns is essential when evaluating patients with unexplained upper tooth pain, temple headaches, facial pressure, or periorbital discomfort, especially when dental and sinus examinations are normal. Recognizing the temporalis muscle as a potential source helps guide appropriate diagnosis and conservative, muscle-focused treatment for temporomandibular disorders (TMD) and clenching-related jaw muscle pain.
All images are the copyright of Rich Hirschinger, DDS, Inc., and were created under the direction of Dr. Hirschinger. They may be used by asking permission by completing the form at this page on the gentle jaw website, and they must not be edited. All rights reserved.
Learn about the muscle referral patterns of the muscles that refer pain into the TMJ.
Learn about appliances for TMJ.
Learn about Botox treatment for TMJ and TMD.
