What is Sleep Apnea?
Sleep apnea is a common sleeping disorder marked by shallow breathing, pauses in breath and labored breathing punctuated by gasping or snoring sounds. Pauses of breath can last from several seconds up to minutes and can happen from five to thirty times or more per hour. A pause may be followed by a choking or snorting sound as the sleeper involuntarily gasps for breath.
The two main causes of sleep apnea are a blockage of the airway and poor signals from the part of the brain responsible for directing the muscles that control breathing. These two causes may occur together, however sleep apnea caused by a collapsed or blocked airway, known as obstructive sleep apnea, is the most common reason sleep apnea is experienced.

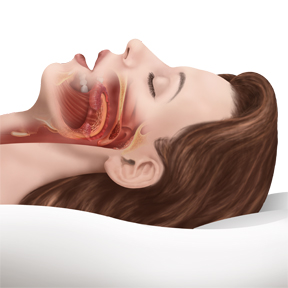
The illustrations on this page were developed by a medical illustrator under the guidance of Dr. Hirschinger.
As oxygen is restricted to the lungs, blood and brain, the sleeper is less likely to fall into deep, restorative cycles of sleep. A person suffering from sleep apnea finds himself or herself tired during the day as the disorder inhibits restful sleep. A lack of quality sleep can lead to accidents or poor job performance. Serious health concerns including heart disease, high blood pressure, stroke, diabetes and depression can also result from untreated sleep apnea.
The condition is a highly manageable one as there are a number of treatment options that can relieve the symptoms of sleep apnea. Treatment options range from lifestyle change such as weight loss and smoking cessation, to devices that keep the breathing passage open through pressurized air or by altering the position of the lower jaw and connected airways, to surgery. An individual with sleep apnea should monitor their condition regularly to ensure symptoms and negative health affects are minimized.
Sleep Apnea Fact Sheet
Sleep apnea is a conditioned marked by pauses in breathing during sleep. A pause, called an apnea, can last between ten seconds to minutes. Pauses can occur five to thirty or more times per hour.
Obstructive sleep apnea occurs when a physical barrier blocks or collapses the air passageway. Central sleep apnea occurs when the brain fails to send signals to muscles that control breathing. Complex or mixed sleep apnea is a combination of both obstructive and central sleep apnea. Obstructive sleep apnea is the most common, making up 84% of cases of sleep apnea.

In cases of obstructive sleep apnea, a pause in breath is often followed by a choking, gasping or snoring sound as air passes through a narrowed or blocked airway. Not all snoring is caused by sleep apnea.
More than 12 million Americans have sleep apnea, according to the National Institutes of Health. More than half of those with obstructive sleep apnea are overweight.
The risk of sleep apnea is higher among males, increases with age, and is more common in African Americans, Latinos and Pacific Islanders than Caucasians. Smoking and being overweight are also risk factors for sleep apnea.
Daytime signs of sleep apnea include sleepiness, morning headaches, morning dry throat, as well as irritability, depression and difficulty concentrating due to lack of quality sleep. Untreated sleep apnea can increase risks of heart disease, stroke, high blood pressure, diabetes, and irregular heartbeat.
Sleep apnea frequently goes undiagnosed because the person with the condition does not notice the signs while sleeping. A person with sleep apnea may wake up in the morning and not know that irregular breathing has occurred during the night.
A bed partner or family member may recognize sleep apnea. Those close to someone displaying chronic snoring and pauses in breath can help that person by encouraging him or her to see a doctor.
A physician through family history, medical examination and the result of sleep studies can diagnose sleep apnea.
There are a variety of treatment options available to someone with sleep apnea. A doctor can help a patient determine if lifestyle changes, dental appliances, a CPAP breathing device or surgery can effectively treat the causes of sleep apnea.
Causes of Sleep Apnea
There are a number of potential causes of sleep apnea, which is often a chronic condition. One kind of sleep apnea is central sleep apnea, which occurs when the area of the brain that controls breathing fails to send proper messages to the muscles that control breathing. This type of sleep apnea is often caused by certain medicines or in people with medical conditions.
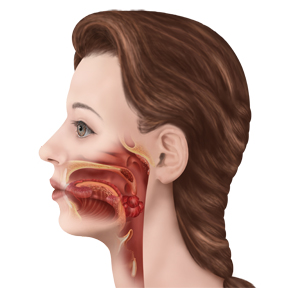
The more common type of sleep apnea is obstructive sleep apnea, which is caused by a blockage of the breathing passage or a collapsed airway. With the airway blocked, it is difficult for air to travel through the airway to the lungs. Pauses in breath occur as the physical obstruction keeps air from traveling freely through the airway. A snoring sound results as air is squeezed through the breath’s obstructed pathway. Not all snoring is caused by sleep apnea, so one should not confuse snoring and sleep apnea although many people who snore do suffer from sleep apnea.
Children with enlarged tonsils are also at risk of experiencing obstructive sleep apnea as the inflamed tissue blocks the breathing passage. Small structural features along the air passage, such as the airways of the nose, mouth or throat, can result in sleep apnea as the small size may serve as obstacles to breathing.
Also, during sleep, the muscles in the throat and along the air passageways relax. Overweight individuals are often affected by obstructive sleep apnea as the excess tissue weighs heavily on the airway, causing it to collapse. According to the National Heart Lung and Blood Institute, more than half of people with sleep apnea are overweight. The condition is also more common in males than females, among those with a family history including sleep apnea, and the chances of experiencing sleep apnea becomes more common with age.
Sleep Apnea Assessment Questionnaire
The following questions are excellent screening questions to determine if you are at risk of having sleep apnea. Please answer the questions and submit the form, and either Wendy or Dr. Hirschinger, who sees patients from Los Angeles, Beverly Hills, and any area outside of Southern California for obstructive sleep apnea, will contact you to let you know if you are at risk for sleep apnea. These are simple screening tools but the only way to diagnosis sleep apnea is for you to have an overnight sleep study at a certified sleep lab, and then have the results read by a sleep physician.
There are many doctors who use dental appliances to treat obstructive sleep apnea but many took a weekend course or two and then started treating patients. Dr. Hirschinger attended a full time, two year residency at UCLA in orofacial pain and dental sleep medicine. Please learn more about Dr. Hirschinger.
Sleep Apnea Treatments
There are multiple methods of managing the symptoms associated with sleep apnea. An individual should work with his or her doctor to find a treatment plan that is effective and comfortable. The goal of sleep apnea treatment is to restore ease to breathing during sleep and to alleviate associated symptoms such as excessive daytime tiredness and snoring. By treating sleep apnea, a patient may also reduce associated health risks including heart disease, diabetes, stroke and high blood pressure. Treatment options include lifestyle changes, breathing devices, dental appliances and surgery.

Some individuals with sleep apnea find symptoms alleviated through lifestyle changes. Sleeping position can have an effect on keeping airways open. Sleeping on one’s side may exert less pressure on the breathing passages than sleeping on ones back. Alcohol and some sleep medications may cause sleep apnea symptoms to worsen by relaxing the muscles that line air pathways, so reducing or eliminating these substances may improve sleep apnea. Overweight sufferers may be able to lessen throat collapse by losing weight. Smokers may find sleep apnea improves after quitting. Some nasal sprays, allergy medicines, or over-the-counter remedies can help keep airways more open during sleep.
Dental appliances or oral appliances may also help relieve the closed air passageways that trigger sleep apnea. A device worn in the mouth controls the position of the tongue and lower jaw, keeping the throat more open during sleep. There are a number of custom-fitted dental appliances that can be made by a dentist trained in sleep apnea that can be worn by a patient who is diagnosed with the disease. An individual should consult with his or her dentist to make adjustments to the device in cases of discomfort, to maintain effectiveness through correct positioning, or if any bite changes occur.
The most common treatment for mild to severe sleep apnea is the continuous positive airway pressure device, or CPAP. This device keeps the airway open by exerting air pressure in the mouth and throat. A constant stream of low-pressure air is blown into the throat via a mask worn over the mouth and nose or more typically just the nose. The air presses the walls of the throat open, preventing collapse or blockage of the breathing passage.
There are many types of CPAP devices, and an individual should consult with his or her doctor to find the combination of mask and machine that works best. A CPAP device may require periodic adjustment and maintenance in order to ensure optimal effectiveness.
Surgical solutions to sleep apnea seek to increase the size of the airway by removing or shrinking tissue or to support the lining of the throat to prevent the collapse that occurs with muscle relaxation. Physically removing the tissue with surgery is one procedure that may be appropriate. A series of shots to shrink excess tissue may also be effective or the air passageway may be supported by a piece of stiff plastic inserted under the tissue. A doctor evaluating the exact cause of an individual’s sleep apnea condition can only determine the procedure most appropriate for a patient.
Life with Sleep Apnea
Sleep apnea can deteriorate an individual’s quality of life by causing daytime sleepiness and contributing to depression, poor job performance, increased risk of accidents and increased chances of additional health risks such as diabetes, heart disease, stroke and high blood pressure. Snoring sounds can also affect family and loved ones of an individual with sleep apnea by interrupting the quality sleep of those around them.
However, sleep apnea is usually manageable through one or more treatment options, including breathing devices, lifestyle changes or surgery. Treatment of sleep apnea can greatly increase happiness, restfulness and health of an individual with sleep apnea and those around them.
A person with sleep apnea may want to avoid gaining weight as weight gain can worsen the condition, while losing weight may improve sleep apnea. If an individual is using a CPAP to treat sleep apnea, weight loss and gain often requires adjustments to the pressure exerted by the breathing device. It may take some time to adjust to the feeling of sleeping with a CPAP, but patients usually report a feeling of relative comfort after a week.
However, it is important to stay aware of ones comfort when using the device and to share observations with the treating doctor. Some side effects of a CPAP include dry or stuffy nose, irritated skin around the mask area, headaches, and stomach bloating. There are many CPAP machines and masks, any one of which may minimize or relieve side effects and improve comfort.
Because a person with sleep apnea is sleeping when the condition occurs, it is difficult for him or her to notice symptoms themselves. Family members or those close to a person with sleep apnea can help monitor the condition by noticing and reporting signs to the individual.
Until sleep apnea is properly treated, an individual with sleep apnea should be aware of the effect of tiredness while driving, operating machinery, and during other tasks that require alertness.
Diagnosing Sleep Apnea
Sleep apnea often goes undiagnosed, as the person experiencing the condition is asleep when the majority of symptoms occur. Doctors cannot positively diagnose sleep apnea during routine visits as an individual must be sleeping for the main indicators to be present. Typically, it is the family or friends of a person with sleep apnea who notice symptoms, such as choking sounds and pauses in breath during sleep, and can report it to the individual.
If a patient suspects they are suffering from sleep apnea, a doctor can check for some secondary symptoms of the condition. The soft palate or uvula may be swollen as a result of irritation caused by snoring associated with forcing air through the compromised airway in cases of obstructive sleep apnea.
A doctor may also be interested in a patient’s family history, as a family history of sleep apnea is a strong indicator of the condition. The patient is also likely to be experiencing daytime fatigue due to poor quality sleep because oxygen is in low supply. If sleep apnea is suspected, an individual can be evaluated in a sleep study.
An overnight sleep study, performed by professionals through a polysomnogram (PSG), measures a number of factors including brain function, eye movement, heart rhythm and respiratory airflow in order to diagnose sleep disorders like sleep apnea. A person with clinically significant sleep apnea will demonstrate blood oxygen desaturation of three to four percent or more, and apneas, or pauses in breathing, of at least ten seconds at a rate of five or more episodes per hour.
