Signs and Symptoms of Neuropathic Pain
The set of orofacial neuropathies includes a spectrum of symptoms, although they are broadly characterized by:
- Sensations of pain, aching, burning, numbness or tingling.
- Pain that occurs in specific or generalized areas of the face, head, mouth or neck.
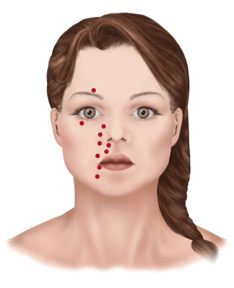
Some neuropathic pain conditions manifest as constant dull pain while incidences of episodic pain have been described as a shock-like burning sensation. Closer examination of several major orofacial neuropathic pain conditions reveals signs and symptoms in greater detail.
Trigeminal neuralgia is experienced as attacks of sudden, severe stabbing pain usually lasting several seconds. Episodes may repeat in succession and occur throughout the day. Attacks are triggered by contact with the affected area, such as the cheek, teeth or scalp. A patient may suffer from trigeminal neuralgia episodes for a period of days, weeks, or months, and then experience a pain-free period lasting months or years. As the condition progresses, it often worsens, and an individual has fewer and shorter periods of relief. A pre-trigeminal neuralgia condition may precede the onset of classic trigeminal neuralgia symptoms. Pre-trigeminal neuralgia, or Type 2 trigeminal neuralgia is felt as a constant aching in an affected region.
Atypical odontalgia is also known as phantom pain syndrome because the defining symptom is a toothache-like feeling. An atypical odontalgia sufferer feels aching pain in a tooth without the presence of an identifiable problem.
Oral nerve injury caused by trauma during medical or dental procedures is marked by constant pain, aching, burning, numbness or tingling in the mouth, tongue or lip. Nerve damage may also result in loss of sensation in these areas.
Complex regional pain syndrome usually affects a patient’s limbs, such as the arm, leg, hand or foot, although it may be experienced in the head and neck area. The condition is marked by continuous throbbing, aching or burning pain; a sensitivity to the touch, cold or heat; a change in skin color, texture or temperature; swelling; muscle spasm or weakness; and decreased mobility of the affected region. There are three stages recognized in CRPS. In the first stage, from the first to the third month, the onset of the above symptoms occurs. During the second stage, from the third to the sixth month, pain and swelling intensifies, hair growth decreases, nails and skin may become dry and brittle, and joints and muscles become stiff and weak. In the final stage, the changes to the skin and bone are irreversible. Muscle loss, limited mobility and involuntary contractions of muscles and tendons may occur.
Neuropathic Pain Fact Sheet
Neuropathic pain conditions are caused by injury or disorder of nerves in the central or peripheral nervous systems resulting in episodic or continuous pain or numbness.
Among the more common neuropathies that affect the head and facial regions are trigeminal neuralgia, atypical odontalgia, and complex regional pain syndrome.
The most well-known and common cause of chronic or episodic orofacial neuropathy is trigeminal neuralgia. This condition is often the result of pressure on the trigeminal nerve by a blood vessel at the base of the brain. Pain from this condition is frequently described as a sudden, intermittent, shock-like, burning sensation.
Atypical odontalgia is also known as phantom tooth pain and mimics the sensation of a toothache without an identifiable pain source.
Damage to the nerves in the jaw may result from dental procedures including tooth extraction, local anesthetic injections and improper implant placement, leading to the onset of a chronic pain condition.
Complex regional pain syndrome, in which continuous aching pain manifests in a localized area, is thought to originate in a dysfunction of the sympathetic nervous system.
Treatments for orofacial neuropathic pain conditions vary based on the underlying cause of the condition, and may include surgical procedures to intentionally damage the affected nerves so that pain signals are blocked. Antiseizure medications may be effective in reducing nerve activity that sends pain signals. Antidepressants medications may also help to reduce pain.
MRI scans, X-rays and CT scans may be conducted to identify nerve damage, although no single test is known to reliably diagnose orofacial neuropathic pain conditions. A detailed medical history and record of patient symptoms is necessary for diagnosing specific neuropathic conditions.
The National Institute of Neurological Disorders and Stroke (NINDS) is the division of the National Institutes of Health that conducts research on neuropathic conditions, causes and treatments.
